Introduction
A
32-question survey designed to assess first year medical students’ knowledge,
experience and attitudes towards psychiatric illness was administered to 424
students from three medical schools in the fall of 1998. The survey was designed to inform medical
training in a period when primary care doctors are often the first medical
professionals to evaluate persons with psychiatric illnesses and to make decisions
about referrals for further treatment. Of
course, the results of this survey do not offer a representative sample of all
first year medical students in the
The medical student survey included questions about
the respondents’ knowledge, personal experience, attitudes and help seeking
behavior with regard to psychiatric and medical illness. The number of respondents from school A, B
and C was 89, 121 and 214 respectively, representing more than 90% of the first
year class at each school. Some
comparisons are made between the results garnered from this sample and those
obtained in a random sampling of 400
Of the 424 medical students surveyed, 47 percent were female and 66 percent were between the ages of eighteen and twenty-four. Thirty percent of the first year medical students were undecided when asked what their planned future specialty was going to be. Of those who did name a specialty, 37% chose primary care or family medicine, 18% selected pediatrics, 20% named surgery or a surgical sub-specialty and 3% listed psychiatry as their future specialty.
Knowledge
The
knowledge section of the survey was comprised of seven question meant to test
the medical students’ basic knowledge of psychiatric illness. Two additional questions about medical illness
were included for comparative purposes. The
knowledge questions were based on common facts that were thought to indicate
the medical students’ initial knowledge of medical and psychiatric
illnesses. The percentage of correct
answers by medical students to the knowledge questions about psychiatric illness
is used to indicate their basic knowledge.
For two of the questions the medical students’ knowledge is compared to
the results of the ODC survey of the general public in
The questions answered correctly by the medical
students most often (Table 1) were awareness of the possibility of significant
improvement of schizophrenic illness (76%) and the implications of depression
for heart disease (72%). The most
frequently missed questions concerned knowing that split personality is not a
feature of schizophrenia (41%) and the success rate of insanity pleas in felony
cases (27%).
Table 1: Correctly answered
questions about psychiatric illness
Knowledge
About Mental Illness
|
Percent
Answered
Correctly
|
|
Significant improvement with schizophrenia
rare |
76% |
|
Depression increases risk of heart disease |
72% |
|
Cycles of moon effect people w/ MI |
67% |
|
Treatment for MI equivalent to medical
illnesses |
52% |
|
ECT considered unsafe and rarely used |
52% |
|
Split personality a feature of schizophrenia |
41% |
|
Insanity defense successful in felony cases |
27% |
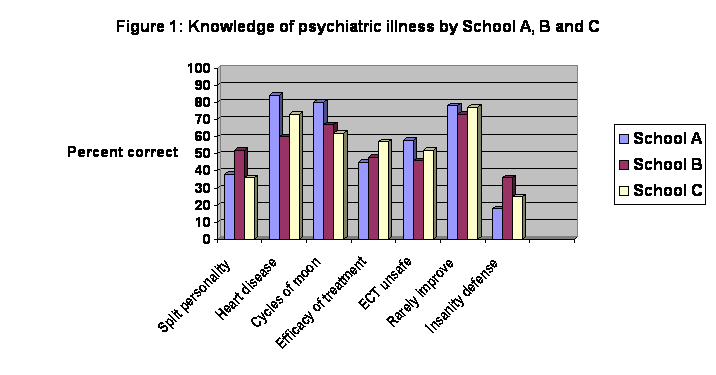
There were only minor differences between
the three schools in the percentage of correct responses to the various
knowledge questions (Figure 1).
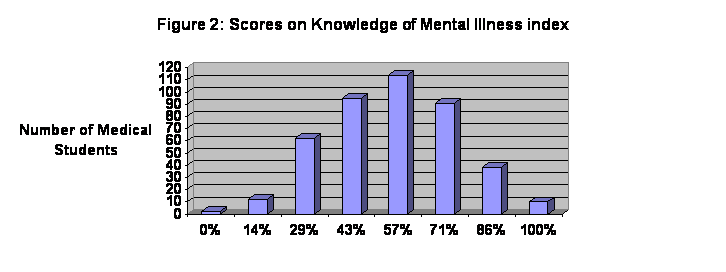
A
‘Knowledge of Mental Illness’ index was created for the percentage of correct
answers to the set of seven knowledge questions about psychiatric illness. The scores form a normal distribution with a
mean score of 57% (Figure 2). Two-thirds
of the 424 medical students surveyed answered correctly less than 60% of the
knowledge questions.
Students
were asked to report on where they think they learned the most about
psychiatric illness. More than one
source of information or learning was accepted for this question. Undergraduate school and personal experience
were the two most common sources of information about psychiatric illness for
these medical students (table 2).
Table 2: Sources of knowledge of psychiatric illness
SOURCE OF Knowledge
|
Percent |
|
Medical school |
4% |
|
Undergraduate school |
43% |
|
Personal experience |
24% |
|
TV and electronic media |
13% |
|
Print media |
21% |
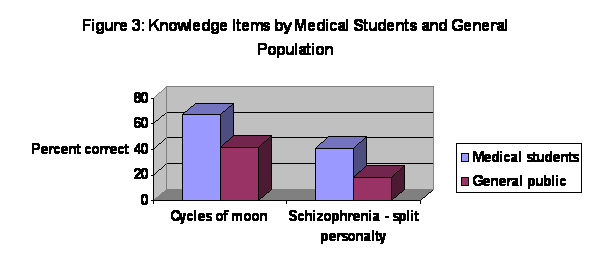
Personal Experience
Medical
students were also asked if they had any personal experience with mental
illness. Experience with mental illness
included either the student having a mental illness or having a friend or
family member who had suffered from a mental illness.
Table
3 lists the percentage of students who reported having firsthand experience
with psychiatric illness either through a personal diagnosis or with friends or
a family member. The students who reported
having personally suffered from a mental illness represented 3% of the total
number of medical students surveyed. Of
the sample, 47% reported having a friend or family member who had a mental
illness. The general
Table 3: Personal experience with psychiatric illness
personal experience
|
Percent
|
|
Respondent suffered from a psychiatric illness |
3% |
|
Friends or family members suffered from a
psychiatric illness |
47% |
opinions
Towards Treatment in Medical Culture
|
Agree |
Neutral |
Disagree |
|
Psychiatric patients receive same medical care
as others. |
20% |
33% |
47% |
|
Slang terms are common in medical culture. |
10% |
14% |
76% |
|
Slang terms are harmless. |
4% |
1% |
95% |
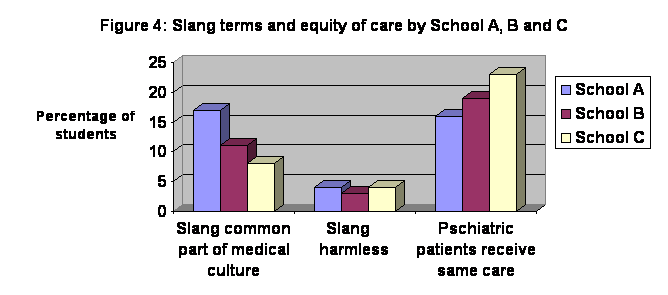
Help Seeking Behavior
In assessing medical students’ help seeking behavior
the same questions were asked with regard to heart disease and mental illness. Students were asked how likely they would be
to seek treatment for the two conditions named.
Table 5 compares the likelihood medical students' would seek treatment
for heart disease and psychiatric illness.
Almost all of the respondents indicated they would be very likely to
seek treatment if they suspected they were experiencing symptoms of heart
disease, while only 46% would do the same in the case of a psychiatric
illness. This disparity suggests there
is greater reluctance or a perceived decreased need to obtain professional care
when suffering from a mental illness.
Table 5: Medical student to
seek treatment for heart disease or for a psychiatric illness.*2
Likelihood
to seek treatment
|
very
likely
|
somewhat
likely |
not likely |
|
If thought had heart disease symptoms |
98% |
2% |
0% |
|
If thought had mental illness symptoms |
46% |
40% |
14 % |
Students
were also asked how likely they think a person would be to tell their employer
about their condition whether that condition is heart disease or a mental
illness. Almost all of the students
responded by saying that a person was not likely to tell their employer about a
mental illness (table 6).
Table 6: Perception of
likelihood person will disclose to employer had heart disease or had a
psychiatric illness.*2
Likelihood
to tell employer
|
very
likely
|
somewhat
likley |
not likely |
|
If had heart disease |
42% |
36% |
22% |
|
If had a mental illness |
1% |
6% |
93% |
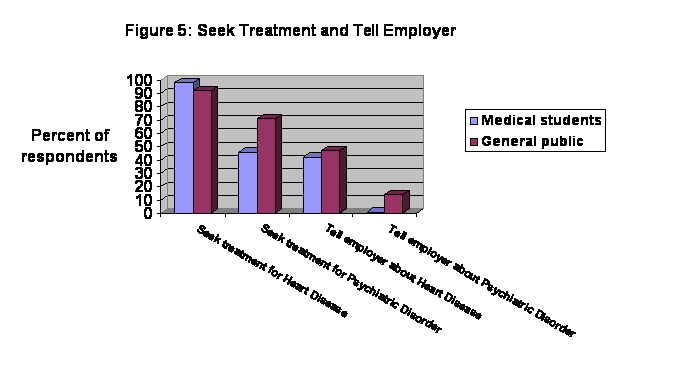
These same questions were asked of the ODC
general population sample. The
distribution in Figure 5 shows the percentage of respondents for the medical
students and the general public who would seek treatment for heart disease and
psychiatric illness and also the number who would tell their employer about
these same conditions. Although over 90%
of the respondents in each group reported they would be very likely to seek
treatment for heart disease, there was a difference between the medical
students and the general population in regard to the likelihood they would seek
treatment for a psychiatric illness. About
25% more of the respondents in the general population than among medical
students reported they were very likely to seek treatment for a psychiatric
illness.
Discussion
The
purpose of this survey of first year medical students at three medical schools
was to obtain a “biopsy” of the knowledge, attitudes and experiences about
psychiatric conditions they bring to their education. It was thought that the results could inform
educational efforts in medical instruction.
On
questions of knowledge, students bring substantial areas of misunderstanding
about psychiatric conditions and treatments to their schooling. Many students endorse popular myths about
schizophrenia, ECT, and the insanity defense, and a substantial minority
endorse a myth about bipolar illness. A
substantial minority lack information about the role of depression in heart
disease, the course of schizophrenia, and efficacy of medication in
psychiatry. Students did do better than
the general public survey on several myths in psychiatry.
One
half of students report knowing someone with a psychiatric condition, including
the 3% who have a psychiatric condition themselves. Students report the most common source of
information about psychiatric illness is undergraduate school followed by personal
experience, print media and electronic media.
Students indicate more learning from formal education and less from TV than
other population surveys.
Students
show a clear pattern of differentiating psychiatric illness from heart disease
in terms of seeking help and determining whether a person with these conditions
would tell his/her employer. These are
findings that may have implications for how doctors advise and create access to
psychiatric treatment as opposed to treatment for heart disease. Notably, many students believe people with
psychiatric illness do not receive the same level of care as non-psychiatric
patients.
These
findings have implications for medical education in relation to people with
psychiatric illnesses. Knowledge
deficits, endorsement of popular myths, and an aversion to seeking help for
psychiatric conditions as compared to “medical” conditions all point to a
substantial need for thoughtful interventions that could include curricula,
exposure to people with psychiatric conditions, and mentoring/modeling in
medical education.
Further study could include a comparison of interventions involving medical schools with different educational approaches, or following a cohort of students to discern the effect of medical socialization toward psychiatric illness.
Footnotes:
1. Agree = response choice (1)
strongly agree, (2) agree; Neutral = response choice (3) no opinion; Disagree =
response choice (4) disagree, (5) strongly disagree.
2.
Very likely = response choice (1) absolutely certain, (2) very likely; Somewhat
likely = (3) somewhat likely; Not likely = response choice (4) not likely, (5)
definitely not.