The Women’s Health Network (WHN), a program of the Massachusetts Department of Public Health, provides screening examinations to income-eligible women for the early detection of breast and cervical cancer and cardiovascular disease risk. The Women’s Health Network breast and cervical cancer program component is funded in part by the Commonwealth of Massachusetts and in part by the U.S. Centers for Disease Control, through the National Breast and Cervical Cancer Early Detection Program (NBCCEDP). The Women’s Health Network Heart Disease and Stroke Prevention Program (HDSPP) is funded by the CDC’s Well-Integrated Screening and Evaluation for Women Across the Nation program (WISEWOMAN). The Department of Public Health administers the WHN and contracts with health care organizations to deliver program services in different areas of the state.
Introduction
Early detection is critical for improving cancer and cardiovascular disease (CVD) outcomes, yet it is of little value when women with problematic test results do not return for further testing and, if necessary, treatment. The Women’s Health Network seeks to ensure that low-income women who do not have adequate health insurance return for timely and appropriate follow-up after receiving problematic test results. Case managers have the primary responsibility for ensuring follow-up, but the WHN case manager is assisted at each of the 26 contracting health care organizations by a program coordinator who manages services and, at many sites, by a client navigator who helps to reach eligible clients. At the six WHN contracting organizations that also offer the Heart Disease and Stroke Prevention Program (HDSPP) services, the WHN service team includes Risk Reduction Educators.
The Women’s Health Network Case Management Evaluation Project was designed to describe the practice of case management as it has developed at the 26 health care organizations that contract with WHN (Contracting Organizations) and to identify the bases for and results of these practices. In this report for the WHN Expert Panel, the analysis of the case management evaluation data is designed to answer five general questions:
(1) What are the characteristics and needs of clients in the Women’s Health Network?
(2) How effective is the delivery of WHN case management services?
(3) What are the impediments to service delivery by WHN case managers?
(4) How do case management practices vary between service vendors?
(5) How do case management practices and case manager characteristics influence service outcomes?
Methodology
The perspectives and characteristics of both WHN clients and WHN staff were measured in separate surveys, while client clinical status and service outcomes were identified through WHN client and service records. The resulting databases were combined for some analyses. Service records were first aggregated to the client level and merged with data on client demographic characteristics available in a WHN database. These data were then merged with data obtained in the phone survey for those clients who were selected randomly for the phone interviews. These combined client records were then aggregated to the site level and merged with the case manager data. These datasets thus allow analyses at the level of both clients and contracting organizations (where the case managers are employed).
The Client Survey
Staff at the
University of Massachusetts Boston Center for Survey Research drew a
representative statewide sample of the 3,178 women who had been identified as
eligible for the case management program within the 12 months prior to
Prior to sample selection, the population was stratified by final diagnosis. The 456 women who had received a diagnosis indicating that cancer was likely were then sampled randomly with a likelihood of selection of .8, while the 2722 women who had not received a diagnosis indicating cancer were sampled randomly with a selection probability of .2. The specific diagnoses that were oversampled (and the corresponding number of cases) were “atypia noted (22),” “cancer identified (90),” “cervical polyps (2),” “high grade SIL (24),” “HPV/atypia (76),” “invasive carcinoma (2),” “low grade SIL (32),” “mild dysplasia (115),” “moderate dysplasia (58),” “severe dysplasia (31),” and “vaginal neoplasm (4).” The specific diagnoses that were undersampled were “normal benign (233),” “cancer not identified (2186),” and “no diagnosis (303).” This disproportionate sampling strategy ensured that most of the women who were surveyed had had multiple contacts with their WHN case manager and were likely to recall the experience. Women being seen only for cardiovascular risk reduction were not included in the sampling frame.
Individual cases were selected on a random basis. Up to 30 phone calls were made to prospective sample members but 23.9% of the sample still could not be located. Of those who were contacted, interviews were completed with 72.9%, yielding a final sample of 207 respondents. Case weights were calculated to adjust for the disproportionate sampling strategy as well as the variability between groups in the survey response rate. For percentages describing the entire WHN client population, the sample is weighted (the reported Ns and the calculations of statistical significance are based on the unweighted sample). The interview schedule was translated into both Spanish and Portuguese. Sixteen interviews were conducted in Spanish and 13 in Portuguese.
Measures
in the client survey included overall health, knowledge of the WHN program,
case management services received and satisfaction with those services, ratings
of potential barriers to follow-up testing and treatment, and satisfaction with
the WHN program overall (see appendix).
Depressive symptoms were measured with a two-question screening index
validated by Haggman et al. (2004) with physical therapy patients.
The Case Manager Interviews
The project research assistants interviewed in-person each of the WHN staff delivering case management services (N=31) for the 26 WHN contracting health care organizations, as well as all but one site’s program coordinator (with one exception), for a total of 51 interviews. The interviews included both fixed-response and open-ended questions. Although work roles often overlapped, at each site the individual who functioned primarily as the site’s case manager was distinguished based on self-reported work activities. The total number of case managers identified was 31, since one of the 26 contracting organizations had multiple service sites that each had staff performing case management functions. For some analyses, case manager responses are compared to those of program coordinators.
Quantitative measures constructed from the case manager interviews included number of work roles, frequency of engaging in particular service and work activities, satisfaction with the program and with the job, and ratings of potential barriers to service delivery (see appendix).
The case manager interviews included many open-ended questions, both as a means to obtain additional detail about responses to the fixed-choice questions and in order to probe for feelings about the program operations. Illustrative quotes from these responses are presented throughout this report.
Service Records
There were 4099
women eligible for case management services for breast or cervical cancer
issues in the period studied (2003 and 2004 prior to
Service utilization and outcomes were obtained from the program’s service database for all of these 3,178 clients. Records of services received by these clients within the preceding three years were added for this group (the earliest service date for the data obtained was July 2001). The resulting 10,417 records of service visits for the case managed clients were aggregated to the level of the individual client. These aggregated records of service visits were merged with the records containing background data on the 3,178 clients.
This process of aggregating service data and merging it with client background information was repeated for clients whose service records included visits for CVD services at one of the six contracting organizations offering the HDSPP program. The entire service database was then aggregated again to the client level and clients were classified by service type in terms of the last services they received during the period studied. This resulted in a total service database of 3282 women, of whom 2523 were last seen for breast cancer issues, 643 were last seen for cervical cancer issues, and 116 were last seen for CVD services (of these, 101 women had been seen only for CVD services during the period studied). For some analyses concerning the organization of services, the six sites that offer HDSPP (CVD) services are distinguished from others.
Two measures were selected from the service database to indicate timeliness in service delivery: time from the triggering event to diagnosis and, for the 357 clients who received treatment, time from diagnosis to treatment. The total number of medical visits is also used in the analysis.
Service records were matched with the phone survey data for the analysis of relationships between service history and client perspectives. Service records were also aggregated to the site level and merged with the case manager interview data file in order to allow analysis of the relation between case manager perspectives and characteristics and client service experience.
In different analyses, WHN sites are distinguished by region (there are seven) and by type of organization: centralized medical sites (such as local hospitals), decentralized medical sites (with several physical service delivery sites), community health centers and one large hospital-based collaborative.
Measures constructed from each dataset are listed in the Appendix. Almost all multi-item scales achieved an acceptable inter-item reliability coefficient (Cronbach’s α) of .70 or higher. Fixed-choice questions in the case manager interview were supplemented with open-ended questions. Responses to the open-ended questions were coded and summarized and are used in this report to illustrate particular service issues.
The Contract Manager Interviews
At the start of the case manager study, the project research assistants interviewed in-person each of the three WHN staff who manage contracts for the 26 health care organizations providing WHN case management services. The interview distinguished large, multi-site contractors from smaller contractors, and those that were performing well from others facing significant challenges. The goal of the contract manager interviews was to learn more about the different types of contracting organizations and the issues they faced, rather than to measure characteristics of each contracting organization through the contracting manager. In addition to questions about adherence to the WHN contract, the interview schedule included questions about case management operations, the role of non-case management staff, and relations with clients and WHN medical service providers. Insights from these interviews are included in this report when they add to data obtained from other sources or when they help to emphasize the importance of key findings.
The
Findings
In this section, background information is presented first about WHN clients and case managers, including the health of clients and the services provided by case managers. Evaluative data on WHN service delivery is then presented from both the client interviews and case manager interviews. These data are organized by topic and include, as available, quantitative data from the client phone survey and both qualitative and quantitative data from the case manager interviews, as well as a summary of the contract manager interviews. The sociodemographic characteristics of all clients in the service database are presented in this section, for comparison with the characteristics of the phone survey clients, while service outcome data are analyzed in a later section.
WHN Clients
The client phone survey assessed client experiences with the WHN program as well as their overall health and social characteristics (residential and work status). Client race, primary language, education and age were obtained by matching the phone survey data with WHN service records.
Socio-demographic
Characteristics
WHN clients surveyed by phone were 47 years old, on average; about 20% were under the age of 40 and 10% were 60 years or older (table 1). These figures were very similar to those for the total population of WHN clients seen for breast or cervical cancer issues, from which the phone sample was drawn. Clients seen for cervical cancer issues tended to be much younger than those seen for breast cancer issues, while those receiving CVD services tended to be considerably older.
Table
1
Client Age by
Last Service Issue
|
|
Breast |
Cervical |
CVD |
Total BCC |
Phone |
|
|
Age |
20s |
5.5% |
45.5% |
0% |
13.6% |
10.5% |
|
|
30s |
9.6% |
14.3% |
0% |
10.5% |
9.9% |
|
|
40s |
39.3% |
21.9% |
19.0% |
35.8% |
33.0% |
|
|
50s |
30.9% |
13.5% |
35.3% |
27.4% |
36.6% |
|
|
60s and higher |
14.7% 100.0% (2523) |
4.8% 10.0% (643) |
45.7% 100.0% (116) |
12.7% 100.0% (3166) |
10.0% 100.0% (207) |
Sixty-one percent of the WHN clients surveyed were white, 6% were black, 29% were Hispanic (almost all identified themselves as white) and 3% were Asian or Native American (table 2). These proportions are similar to the racial and ethnic distribution of the population of WHN service recipients receiving breast and cervical cancer services. Women receiving services for cervical cancer issues were more likely to be white than those receiving services for breast cancer or CVD issues.
Table
2
Race/Ethnicity
by Last Service Issue
|
|
Breast |
Cervical |
CVD |
Total BCC |
Phone |
|
|
Race/Ethn. |
White |
54.0% |
70.8% |
48.3% |
57.4% |
61% |
|
|
Black |
7.5% |
4.9% |
5.2% |
7.0% |
6% |
|
|
Hispanic |
36.4% |
22.5% |
40.5% |
33.6% |
29% |
|
|
Asian, Other |
2.1% |
1.9% |
6.0% |
2.0% |
3% |
|
|
|
100.0% (2494) |
100.0% (636) |
100.0% (116) |
100.0% (3139) |
100.0% (203) |
The primary language of almost one-third of the phone sample was not English. Speakers of Spanish and Portuguese each represented 13% of the sample, while 63% were English speakers (table 3). Women receiving WHN services for cervical cancer issues were more likely to be English speakers and less likely to be Spanish speakers than those receiving breast or CVD services.
Table
3
Primary
Language by Last Service Issue
|
|
Breast |
Cervical |
CVD |
Total BCC |
Phone |
|
|
Language |
English |
52.8% |
72.7% |
52.6% |
56.9% |
62.8% |
|
|
Spanish |
24.1% |
14.4% |
31.0% |
22.1% |
12.6% |
|
|
Portuguese |
15.6% |
8.7% |
7.8% |
14.2% |
12.8% |
|
|
Other |
7.5% |
4.3% |
8.6% |
6.8% |
11.8% |
|
|
|
100.0% (2479) |
100.0% (634) |
100.0% (116) |
100.0% (3113) |
100.0% (203) |
Almost two-thirds of the sample had no more than a high school degree, but another 28% had completed some college and 8% had earned a college degree (table 4). Clients with less than a high school education were underrepresented in the phone sample. Women seen for CVD services tended to have less education those seem for breast or cervical cancer issues, while those seen for cervical cancer issues tended to have somewhat more education than women in the other two groups.
Table 4
Education Completed
|
|
Breast |
Cervical |
CVD |
Total BCC |
Phone |
|
|
Education |
Less than High
School |
28.9% |
19.3% |
38.1% |
29.0% |
10.9% |
|
|
High School |
38.1% |
45.1% |
37.2% |
39.5% |
53.9% |
|
|
Some College |
21.7% |
23.9% |
15.1% |
22.1% |
27.6% |
|
|
College Degree |
11.4% 100.0% (2333) |
11.6% 100.0% (594) |
9.8% 100.0% (113) |
11.4% 100.0% (2927) |
7.6% 100.0% (192) |
Forty-four percent were married, while 32% lived alone. Almost half were employed and/or attending school part-time, while 24% were working or attending school full-time and 30% were neither working nor attending school (table 4). (No comparative figures are available from the total population.)
Table
4
Work
&/or Student Status
|
|
Table % |
|
|
Status |
Not Working or Student |
29.9% |
|
|
Part Time Work or Student |
45.8% |
|
|
Full Time |
24.3% 100.0% (205) |
Overall Health and Health
Care
Just over half of the sample rated their health overall as excellent or very good, while about 20% rated their health as only fair or poor (table 5).
Table
5
Self-Reported
Health
|
|
Table % |
|
|
General health |
Excellent |
19.1% |
| Very good |
33.3% |
|
| Good |
27.7% |
|
| Fair |
13.8% |
|
| Poor |
6.1% 100.0% (207) |
|
Half of the clients interviewed reported physical health problems in the past year (table 6). One-quarter said that their physical health problems had affected their daily activities.
Table
6
Physical
Problems
|
|
Table % |
|
|
Physical Health Problems Affect in
Past Year |
None |
52.9% |
| Yes, No Affect on Daily Activities |
24.7% |
|
| Yes, Affected Daily Activities |
22.5% 100.0% (205) |
|
Symptoms of depression were common, with 42% of clients reporting that they had been bothered “by feeling down, depressed or hopeless” or “by little interest or pleasure in doing things” in the past month (table 7).
Table 7
Symptoms
of Depression
|
|
Table % |
|
|
Symptoms of Depression |
No symptoms |
57.6% |
| One symptom |
11.4% |
|
| Two symptoms |
31.0% 100.0% (207) |
|
At the time they were surveyed, 44% reported having some type of health insurance but half said they had not been able to get some medical care they needed within the past two years due to cost. Eighty percent reported having both a usual health care provider and a place where they usually received health care.
WHN Case Managers
The social backgrounds of the 31 Women’s Health Network case managers were relatively homogeneous: thirty spoke English as their primary language, although five said they could communicate in Spanish or Portuguese. All but two of the case managers were white and all but three were at least 40 years old. Twenty-nine case managers were RNs and six of these held Advanced Practice degrees.
The Work of Case Management
Case managers worked an average of 10 hours per week in their case management role and an average of another 10 hours in other roles for the Women’s Health Network, including program coordinator, client navigator, outreach worker, risk reduction educator (in HDSPP sites), and billing and enrollment specialists. Case managers worked an average of three roles for WHN, with 16 working one or two roles and six working five or more roles. A quote from one case manager illustrates the high level of commitment to these roles.
We
are all paranoid about losing a patient or not doing … not doing well. Our philosophy is that it is a sister or
mother … whatever – each patient- so that we care for them the way we’d want
our family member [to be cared for].
Most case managers interacted frequently with their program coordinator and client navigator, when they were not themselves responsible for these roles. Many case managers commented that interaction with other WHN service staff and with medical providers, as well as the resources available in larger health care settings such as hospitals helped in managing work tasks.
There
are many different avenues to go to. …my
program coordinator is full of knowledge and …then I can go to other case
managers if I have a question….
Because
our program is hospital based it is easy for me to coordinate, and plan
services with our providers.
The
providers are all very affiliated with our organization so…. they know each
other … the doctors know each other, they know the program. They know me. I
know their staff.
There’s
three and they are all GYN practices that I have contacts with--the nurses up
there--and it makes a big difference when you get to know them and you’re
talking to them and they get more comfortable with you as well … we work very
well back and forth.
I
think we have such a strong team of physicians who have contracted with us that
it makes it easier for us because between the physicians and their staff they
are very willing to help us.
Others
reported that constrained resources, including unavailability of staff in
related roles, limited their effectiveness.
They’re
hindered by a system that is overloaded. They need more than our little health
center can actually give them and which has really dried up the funding on many
different programs.
I
think that being a healthcare provider within the hierarchy of healthcare
providers and in a program that’s contracted with specialists who have kindly
agreed to take a small payment versus being an advocate, that’s extremely
challenging.
Doing
Women’s Health Network case management is not an easy thing; partly because of
the patient population that you are working with, you’re also serving and
working in conjunction with the physician or the medical provider. You are also serving a master at DPH who
wants things done certain ways and, unlike most other medical case management,
you are also dealing with this whole financial issue.
This
woman that we used to be able to afford to pay a few hours a week also spent
time every month balancing what we paid out versus what we billed. She could do that accounting piece and for
the period of time that she was with the Program we were never in better
shape. We actually knew, you know,
things balanced. We get this amount of
money a month. We are putting out this
amount. That’s not happening as well
anymore because frankly I don’t have the time.
So now that you’ve got me going.
A lot of pressure is from billing problems. Problem bills, not being able to balance
books because we just don’t have the time… it’s an ongoing problem. I’ll tell you really when we had enough money
to support the program and a lot of that money was coming from supplemental
grants. We had a Smoking Cessation
Grant. We had an Outreach Grant through
the American Cancer Society. We were
never in better shape. We had a Program
Coordinator who worked 25 hours a week.
We had me as a Client Navigator that worked 37½. We had a 30 hour a week Outreach Worker who
supported me. Um … our numbers were the
best and we, you now, we were hitting our case load. We can’t do it with this amount of money. We can … it’s a real struggle.
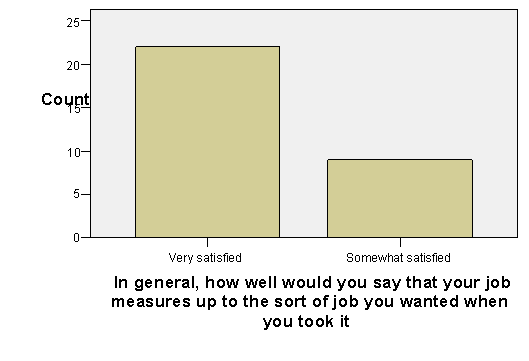
Overall, all case managers were very or somewhat satisfied with their jobs and almost all (90%) found the job very or somewhat like the job they wanted (Figure 1. Most (82%) rated their different job responsibilities as complementary, rather than conflicting. Many respondents expressed a high degree of commitment to the work and to the women served.
Figure 1
Overall Satisfaction with the Job
I think because nurses really do have a
vision for the whole patient because of the training that that we have gone
through. My experience speaks volumes
to what I bring to this program. I couldn’t imagine delegating this to somebody
else. I mean I’m not an expert on
breast cancer so I know my limitations and I think as nurses we do know our
limitations. Cervical stuff I can speak,
you know, forever about … but I know where I can refer this woman so that she
will get the best care. I have another
nurse that … that I can refer her to that is also a breast cancer survivor so I
have really good resources”
…is a special circumstance-registered nurse,
I think she can afford to work here. If
she couldn’t we would have lost her.
It’s been that stressful for her.
You know, there was a time when we could only pay her for 4 hours per
week and then it went to 6 and now she feels it is luxurious to have 7½ to 10.
Our doctor…is working for $50/hr and she has been doing that for this program
for years. … she has said before she
would probably do it for free. That’s
an unusual woman.
Case manager ratings of particular job components varied widely. As indicated in figure 2, relations with other staff in the WHN program—supervisors, coworkers, and contract managers—were the most satisfying aspects of the job components—while salaries and the job in relation to expectations were the least satisfying.
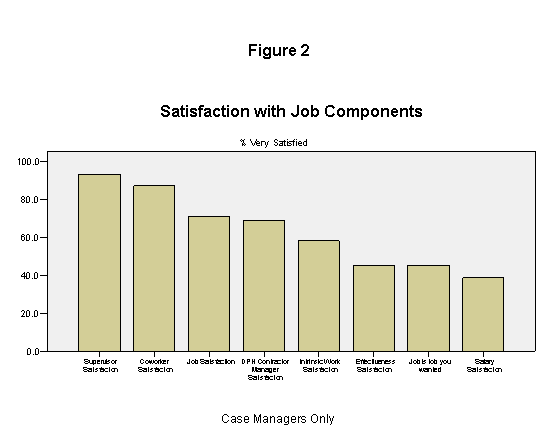
At WHN health care organizations that contracted to deliver only breast and cervical services, through the Breast and Cervical Cancer Early Detection Program (BCCEDP), the average number of active clients in a case manager’s caseload per month was 14, but at the sites that also provided Heart Disease and Stroke Prevention Program (HDSPP) services, the average active caseload was 24 (table 8). Case managers at HDSPP sites also reported adding more clients to their caseload each month and interacting with more clients both by phone—the most common method of communication with clients—and face-to-face.
Table 8
Mean WHN Clients, Past Month by Site Type
|
Number |
BCCEDP |
BCCEDP & HDSPP |
|
Active DPH Caseload |
14 |
24 |
|
Added to Caseload |
7 |
11 |
|
Phone Conversation |
14 |
17 |
|
Face-to-face |
6 |
12 |
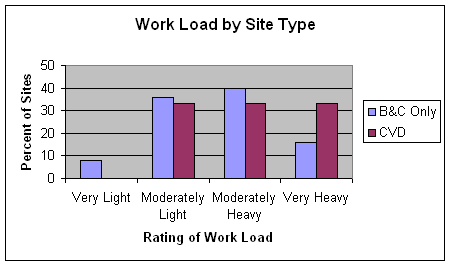
Many case managers rated their workload as moderately or very heavy (figure 3); some described how they tried to manage their own time to ensure completion of work duties.
Only
having basically 2 days to do the WHN. …it means that you have to be very
organized and know ahead of time what you are going to have planned for that
day. Interruptions can throw things very
off whack.
At sites that delivered HDSPP (CVD) services, more case managers reported that their workload was very heavy (figure 3).
Figure 3
A comment by a case manager at one HDSPP site helps to explain the basis of the perceptions of higher workloads at sites that offer both the NBCCEDP and HDSPP programs.
I think, especially with the
cardiovascular, the breast and cervical like they … they start …. They end and
then they go into regular recall; the octopus is the cardiovascular and that
case load just continues to grow plus you have your more acute breast and
cervical. We’re trying to find a way to
… to split it now so that it’s not so overwhelming for … with the feeling of
being overwhelmed and not able to do the job as well as you would like it to be
done. ….. The other part, I think we’re
okay – the breast and cervical but cardiovascular I’d like to see somehow to
manage that more comfortably.
Some case managers reported that their workloads were so heavy that they were forced to spend less time on less essential services like educating clients.
it is very difficult to try to
do the education when you know your case load is just so overwhelming … Um ..
but and that’s why I say moderately because it’s like you want to do and I
think I do it well but then again it’s like you really can’t be on the phone
and spend that time with every single patient …. so ….
The work load has increased
recently and so I have limited time to … um … to be able to look up the results
and that sort of thing so I’m trying to balance that and that is pretty
difficult at this point.
Case managers also reported that the workload of some other WHN personnel could be excessive.
we have a financial aid
counselor but it’s a 9-5 job, so if our patients were coming in at night and we
know they don’t have insurance, there is no one to sign them up. That one financial aid counselor just has a
huge workload and she is trying to check on people who have signed up and
haven’t returned the required documents fully you know to complete their
application and then everyday you still have new people coming up to you
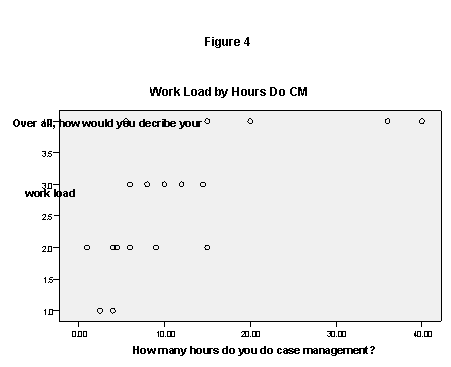
As indicated in figure 4, case managers’ ratings of their workload as moderately (3) or very heavy (4) also rose with the number of work hours they reported spending in their case management role (r=.66). Following up on clients was reported to be very time consuming, and some felt the scope of the case management role was increasing.
it
is hard to …to carry a large load where they have to follow-up on, and in
reaching the clients, you know, and if you’re only here for a couple of days a
week – trying to reach is very hard …. ….I think that that is one of the major
challenges.
It’s a very time consuming job
…. A tremendous, tremendous amount of detail.
A tremendous amount of requirements and more keeps being added and we’re
not getting really more funding for the added role …. you know, the added
things that we have to do. I am sure
you’re hearing that from every single site.
In some cases, feelings that the workload was too heavy was due to the demands made by working with multiple programs and by feeling responsibility for helping clients even after they have received a diagnosis.
Yeah, I’m doing the job
now. So that’s huge. I’m doing it and like I said I can’t devote
everything I’d like to that position. I
look at what [an
I envision…the workload ….over
time becoming pretty tremendous because of the issue of you … as a nurse …
wanting to … wanting to continue to case manage people beyond WHN….. …. I mean fortunately again we’ve been very
fortunate in that our numbers of cancer diagnoses have been very …. relatively
low …. but as we’ve increased our numbers for this year, by definition, I’m
presuming we are going to pick up more cancer diagnoses and how that’s all
going to play itself out I don’t know
Some case managers focused their complaints about insufficient time on the documentation requirements.
The
challenges are the documentation and the restrictive nature of the definition
of case management.
The
paperwork that is required does not benefit the client. I haven’t quite figured out who it benefits.
We, you know, have our own way of tracking our own patients and what care that
they should get. I feel like it’s in addition to the real case management that
we do.
Services Provided by Case
Managers
The client service activities in which case managers most often engaged on a daily basis were tracking test results, finding and connecting with clients and assessing their needs, and educating clients and monitoring their progress (figure 5). The service activities that begin and end the WHN service process-- learning that a woman needs case management, contacting medical providers about treatment, and arranging for discharge—were less commonly reported as occurring on a daily basis, but often took considerable efforts.
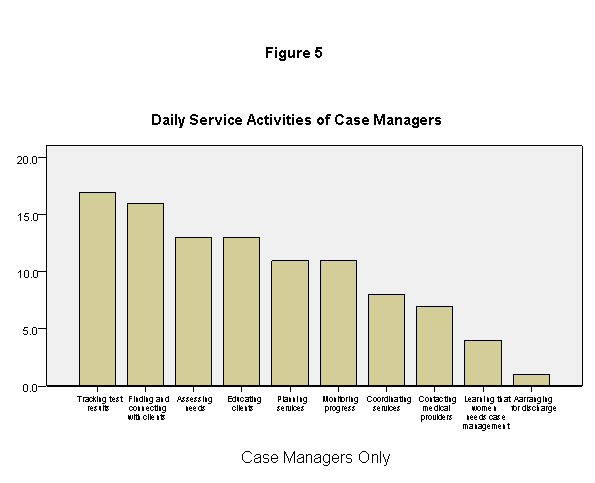
Case managers engaged frequently in both “finding and connecting with clients” and “monitoring their progress” (figure 5). Although almost all case managers felt that most service activities were carried out very well, they gave these two areas relatively low ratings. One less frequent activity, “arranging for discharge,” was also given a relatively low quality rating (figure 6). The case managers and program coordinators made many comments that helped to clarify the bases for this variation in ratings.
Figure
6
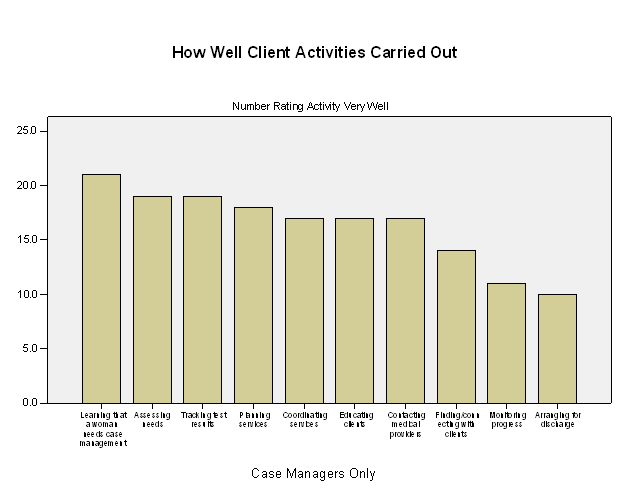
Finding
Clients and Maintaining Contact
Many case managers’ comments referred to the difficulties encountered in maintaining contact with clients. They cited several different bases for these difficulties, including client mobility and lack of client interest.
Lots
of time I’m following-up to get people rescheduled. And for some reason some patients seem to
take several attempts. Other patients
even though they are supposed to call me with the date for their diagnostic
forget and I need to call them and find out when they are scheduled. Sometimes I have to call them afterwards too.
Finding, connecting with clients – I need to follow-up with them and I can’t
find them. I would say that probably
happens with a good 50% of our clients.
They change phone numbers, changed address – out of the country. I’d say that happens every week.
Problems of maintaining contact were frequently due to residential mobility, sometimes in conjunction with ties to another country.
Patients move a lot, change phone
numbers, live with extended families. There are people who disappear. We have a large moving population, we’ve
called and they’ve moved to Puerto Rico, we’ve called and they’ve moved back to
Brazil
Most
of our clients are very transient. So we try to get more than one phone
number and address to contact them or have them call us. The follow up is very
difficult
We have what we call our
frequent fliers – they come to the country for six months, they leave for three
months and they come back for six months.
For us,… language barriers, transient population, people who move, people
who go back to their country for six months or a year then come back and uh mm…
resurface, they changed their names they got married, they changed their
addresses, those are all challenges.
Clients who were in stressful personal situations, including homelessness and abusive relationships, sometimes did not seem to be interested in medical follow-up.
Patients
that are homeless, and don’t want to follow a stringent follow up care, this
and that and is not…. and we can not badger people into wanting treatment care
and at some point an assessment needs to be made, and a capable staff can make
that.
You know, an example of a woman who is living in an
abusive relationship; that’s a fine line that you’re walking,…. trying to
help and navigate through the system; not only help her navigate the system but
you’re navigating, you know, her, and where she is.
Some case managers felt they were successful in keeping in touch with clients, but the effort involved required much time.
Follow-up,
getting in touch with patients… I’ll call them, I’ll send out letters, and then
I’ll send out registered letters. And if
I haven’t had any response within a month then I just take them out. They are basically lost-to-follow-up. And sometimes they’ll come back to the
program and then ding I’ll nab them.
…
It makes you more attuned to keeping track of patients. So these are people
that I really follow closely to make sure things are done.
Monitoring Progress
Monitoring
client progress could be difficult due to requirements of medical providers as
well as due to inadequacies in information technology systems.
The
challenges as I’ve mentioned about working with the neighborhood health centers
is that they [the patients] may be getting their Pap smears at another health
center, – how can we get that
information so that we can put it into AIS so that Women’s Health Network will
give us credit for the fact that they had their pap smear? The tricky thing about site is that we are
really, if you will, the Women’s Health Network is really a Tertiary Care
Center
…the
difficulty of getting the clinical software to interface with the billing
software, which is also the registration software’s challenge...clinical
software and find out like the number of mammograms we’ve done for you know a
certain cohort of women.
Case
managers and program coordinators had developed a variety of strategies to
monitor client progress, including calendars, tickler files, and computer–based
strategies.
The
number one thing has been the whole calendar system – that is allowing us to
stay on top of it-since January. It’s also an evolution of the program
too. It might have worked initially to
develop this program, to make it available.
But it grew into something that works better this way.
They
weren’t sending me information so I stopped paying them. And when they found
out that, you know, they were linked, suddenly, whenever they send me a bill
they send me a copy of what they’ve done. So, I get the bill, I get the office
note, I get any path reports, etcetera.
It’s
really knowing when the woman has gone so we can actually retrieve the results.
And/or teaching providers to automatically send them to us. And strategies? Just education and reiterating the importance
of timely results.
I
have identified certain key informants in each of these areas like a nurse
practitioner who does work with the practice, and I can e-mail and say: so and
so were seen today, was she seen? She will go find the notes or scribbles, talk
to the provider and get an e-mail right back, saying: she [the patient] actually
did not come. So, you may want to give
her a call or something like that.
Arranging for Discharge
Arranging for discharge was one of the less common tasks, but sometimes was difficult due to the program expectation that clients would be discharged from WHN case management when they entered treatment, rather than when their treatment was completed.
Because
I just follow-up when I get the dictation from the doctor saying what they
need, what their follow-up is and I keep a list so until I have checked it off
I know I haven’t received the dictation so I keep hounding them and once they
say what the follow-up is, we make a phone call to the patient so that she is
aware of what the follow-up is and I close her out in case management.
The
difficulty is that you have to discharge the patient just when she needs you
most, when she starts treatment.
Organizational
Tasks
Documenting services was the only organizational task carried out daily by most case managers (table 9). Other organizational tasks were carried out at most sites between a few times a month and a few times a week. Documenting services, seeking advice, and staff meetings were all rated as being carried out very well by almost all sites, but training about work, supervising staff, and evaluating service provision, which were engaged in less frequently, were rated as not being carried out as well at many sites. Respondent comments illustrate some of the reasons for these ratings.
Table 9
How Often
and How Well Organizational Tasks Carried Out
Average Ratings
|
Organizational
Task |
How
Often* |
How
Well** |
|
Documenting
Services |
3.8 |
3.6 |
|
Staff
Meetings |
2.7 |
3.6 |
|
Seeking
Advice |
2.6 |
3.8 |
|
Supervising
Staff |
2.5 |
3.4 |
|
Evaluating
Services |
2.3 |
3.3 |
|
Training |
2.3 |
3.2 |
*1=Never,
2=Few Times Monthly, 3=1-4 Times Monthly, 4=About Daily, 5=More.
**1=Not
at all, 2=A little, 3=Moderate, 4=Very Well.
Documenting services includes such activities as obtaining client consent and recording abnormal test results and tracking subsequent testing until questions have been resolved and the client is either diagnosed with cancer or returned to a routine rescreening schedule. Patients are formally discharged from WHN case management when diagnosed with cancer, but many case managers continue to work with these women to ensure not only that they enter treatment, but also that they continue treatment. Case manager’s and program coordinator’s comments reflected overall satisfaction about documentation, but some frustrations with the paperwork involved.
You have a full record of everything that happened, the sequence it
happened in, and the response to each event.
And it’s closed out in the chart as completed – as no cancer, as
whatever.
Shuffling through the
paperwork … that’s a challenge; and just staying on top of everyone that’s
going everywhere because everyone is heading in a different direction – to a
different surgeon, to a different doctor.
There are different, you know, we have to make sure that our follow-up
is documented and that we have a way to retrieve it, you know, on time.
Like okay for the case management plans, we don’t really have one in
effect, using a form specifically. And
it’s been kind of vague. DPH has said you know you could use this if you want
to, whatever. And because I’m not the supervisor
I don’t pick one and tell them to use it.
It’s really up to them. Because they are the case managers, they are the
ones to decide the best way to run their own case management.
A key issue in the documentation is obtaining client consent. For obtaining consent, the WHN programs use a number of strategies, including having forms in additional languages, adapting the form to their own agency’s paperwork, enlisting outreach workers, and conducting “in-reach” within their own financial counseling staff. Frustrations occur when the amount of paperwork or types of questions asked seem to keep women away from screening.
We keep a log of all
patients that enroll and then when we send out the consents we explain it over
the phone that there is going to be about 8 pieces of paper; so it’s good, you
know, explanation at the time of enrollment.
The paperwork involved in
it is ridiculous.
Well, obtaining client
consent is difficult. Um … because they
will discuss with you over the phone if they want the procedures and yet they
will come in without having consented – signing a consent – so how we’ve
addressed it is we mail out all our forms initially and we put in a
self-addressed stamped envelope for them to return the forms to us and that has
brought this up to a somewhat adequate.”
We actually, the women here, the staff here go to the women, and
enroll them. They are right there on the spot to sign. The service is not
provided until we get the signed consent, so we just don’t do it, without it.”
Getting income verification is difficult, can be difficult… You know, I
tell my staff that it is not up to us, to… you know start digging around to
find out if people are telling us the truth or not. If somebody is going to tell you something we
have to take it as face value. We can’t accuse people of not being truthful
with us.
For tracking the women’s progress through testing and into treatment, case managers used a variety of documentation strategies including computer-based systems, tickler files, and written notes in the charts. Case managers had independently created systems in their own sites that combined the required DPH and CDC forms with resources and requirements of their agencies, as well as those of other programs that support breast and cervical cancer screening and case management such as the Avon Foundation. In some cases these methods were perceived as adequate.
We have a good medical
records department and we have charts when we need them.
Some sites supplemented formal evaluation programs with direct feedback from the clients.
I’m talking to the clients like how did your surgical consult go, or how did the biopsy go, how did the colposcopy go. So I’m always getting feedback from the client
Sometimes the patient will say you know ‘I really don’t want to go back to that particular physician. Then there’s no problem, we just schedule with somebody else. But you know I don’t ask them how they liked their service.
For some case managers, however, documentation requirements were viewed as troublesome or poorly supported.
The
paperwork that is required does not benefit the client. I haven’t quite figured out who it benefits.
We, you know, have our own way of tracking our own patients and what care that
they should get. I feel like it’s in addition to the real case management that
we do.
The computer access
really makes it easier.
Some of our systems are
really old. You know, and they can’t
afford to update so we try to make do with what we have.
I don’t even have a
computer at the moment; we have to share.
There are two in here but there are two other women in here and my job
is usually, remember I said I always work at least 32 …. If I have to stay at
night to use the computer that’s what I do cause at least it’s quiet.
Case managers were open to improvements in information management and looked forward to simplified systems:
It’s a new form for us
but I think that we can provide better documentation with it. Very well; if anything we are double
covering ourselves because we are still tempted to write in the narrative as well
as put it on the worksheets.
I guess the whole ACE
process and the billing process; it is so much better than it was. …going
web-based will be a relief. So I am looking forward to that.
Staff Meetings
Case managers, program coordinators, client navigators, and other program staff work in various combinations, sometimes with individuals sharing roles, and, at other times each position staffed by one person, although often in limited hours weekly. Consequently, few sites reported having regularly scheduled meetings, but many respondents commented about the importance of meetings.
When somebody doesn’t come back when you want them to you sort of step
back and have to reflect – did we do enough education with them? Or did we not assess the barriers that may
exist …. … and that’s another thing that we talk about at our monthly meeting.
A couple months ago we had a meeting at one hospital’s breast
center. We asked the health centers and
our staff at the health centers, who refers there to meet with the hospital
staff so they could put a name to a face and they and the hospital could talk.
The breast center could talk about the difficulty they run into referrals with
health centers and health centers could talk to hospital about the difficulty
they have, the patients have when they refer to the hospital. We did the same
thing with another hospital and we are doing the same thing with the third as well. And it is being great!”
If you’re not here to work together you’re not going to produce
together. I’m frustrated. … very
frustrated cause I think that is the biggest, biggest challenge because we are
a three person program. You can’t
even prioritize when you’re not working as a group.
Meeting with staff is very difficult because there is never enough in
the budget to support the amount of staff time that DPH really requires to do
it. So we brown bag and steal staff time, and none of our health centers do
have staff working exclusively in this program. They had other job
responsibilities and it makes it very difficult.
Sometimes opportunities to confer were enhanced by close quarters and overlapping hours:
We’re all in the same
cramped office. That makes it easier cause you’re right next to each other so
it’s hard not to see each other and be able to collaborate.
And the fact that we’re
small it’s easy to kind of talk to people.
We have a good working
relationship – the three of us.
Everybody is accessible.
We’re in the same office, we constantly communicate and … that’s what makes it easy.
Seeking Advice
Case managers and program staff were asked about the ease of getting advice about their work. In general, there was a great deal of satisfaction with access to guidance. For example, staff reported:
I think that the other staff that I’ve worked with, one person in
particular has been with the program since the start, so I know she does a
wonderful job.
I have a strong
support person here so it’s not a problem.
My resources are readily accessible, which is wonderful. I would seek advice from the clinician here
But on the other hand:
I think some staff
members make it somewhat difficult at times
and not as willing or able to share information – maybe lack of the
providers might be a problem.
I’m not the expert on this and [for] the medical director …WHN is not
her concern, the agency is her concern.
And my supervisor is new. He does
not have a medical background.
When asked about relations with DPH staff, the responses were generally positive, but included some criticisms:
We have open
communication, through e-mail, telephone calls, we see them couple a times a
year at the providers’ meetings. So, there is a very open line of communication
there
I feel like a lot of times I email questions and they don’t really get answered…. I just feel like it really takes a long time to just get an answer, to a lot of basic questions
Training about Work
While most case managers had received some training or technical support in Medicaid regulations and general case management procedures (table 10), eight WHN case managers reported that they had not received any special training related to their WHN case management role. Thirteen reported some WHN program training or technical support in risk reduction education.
Table 10
Training Reported by Case Managers
|
|
Any special
training related to WHN case management |
Training or technical
support in Medicaid Treatment Act |
Training or
technical support in case management procedures |
Training or
technical support in risk reduction education |
Training or
technical support for any other services |
| Count |
Count |
Count |
Count |
Count |
|
|
Yes |
23 |
26 |
27 |
13 |
14 |
|
No |
8 |
5 |
4 |
17 |
15 |
|
Total |
31 |
31 |
31 |
30 |
29 |
When case managers and program coordinators were asked about the adequacy of training about work there were a variety of responses. Some considered the quarterly DPH meetings as meetings, and others referred to these as trainings. Nonetheless, many emphasized the need for training to optimize efficiency in team functioning:
Really what I think is key is teaching all staff about what is expected
for each woman coming through the program.
So anyone can pick up a chart and say she didn’t have blood work, I
wonder why, let’s look back, did she maybe not want it, had she just had it,
did she want it and it didn’t get ordered for one reason or another, well let’s
call her and discuss this – put every scenario that you can think of, all of
our staff are trained and know how to do that and I think that’s a lot is to
give really comprehensive care-we are a total team
Some agencies used creative approaches to provide training.
Once again limited resources, so
we usually provide trainings, in-house trainings, that usually I’ve conducted
b/c well b/c I’m free and well we don’t have to pay me to do other than my
regular salary but its tough to coordinate outside people to come in and do
trainings b/c we just don’t have the money to pay them.
Usually, I’m the one
doing training but now that we have
Some interviewees emphasized the need for more training opportunities.
I was not trained for
this position. I was put into this
position with no training whatsoever.
Nobody knew how to do it. How about a Women’s Health 101? You know, I mean it’s trial and error; fall
on your face, get back up and try it a different way. I mean even to get into the computer they
have class so you know how to get in, you know how to use it. They have a touch-base person but as far as
what is your real job, how do I do this.
And the barriers are that there is so much to learn in detail. And it changes so often, that they just got it down and DPH changes it.
They
are missing the boat on getting
Adequacy of
Work Procedures
Case managers were asked to rate the adequacy of several specific work procedures. Procedures for maintaining client confidentiality, phone access to clients, relations with other providers, and staff cultural awareness and providing timely test results were rated by almost all case managers as “very adequate” (table 11). Ratings were lower concerning the educational materials for clients and for staff, as well as for computer support and the program policy and procedure manual (which had not been completed at the time of the interviews). Respondent comments provide more complete information about these ratings.
Table 11
Average Rating Adequacy of Work Procedures
|
Work
Procedures |
Adequacy* |
|
Maintaining
Confidentiality |
3.9 |
|
Phone
Access |
3.6 |
|
Relations
with Other Providers |
3.5 |
|
Staff
Cultural Awareness |
3.5 |
|
Obtaining
Timely Test Results |
3.5 |
|
Obtaining
Client Consent |
3.4 |
|
Policy
& Procedure Manual |
3.3 |
|
Staff
Educational Material |
3.2 |
|
Client
Educational Material |
3.2 |
|
Computer
Information Support |
2.9 |
*1=Not
at all, 2=A Little Adequate, 3=Somewhat, 4=Very Adequate.
Client Confidentiality
Client confidentiality issues arise around both health care information and the financial information requested. The implementation of the Health Insurance Portability and Accountability Act (HIPAA) has created new regulations for sharing patient information that required new procedures among agencies. The risks of sharing confidential information and problems in reaching clients were also mentioned by case managers and program coordinators as challenges.
Well, you just don’t divulge much
information, you know, like for example trying to contact a patient. I never say why I’m calling. I just say my name, that I am a Case Manager
and could you please have her call me this is my phone number.
Cannot leave a message on their phones--even
using false identities.
They are like ‘oh no you need to call the
patient.’ And I am like I am not going to call a patient that I have never laid
eyes on who has no idea who I am, you know a lot of people in this
community don’t speak English or have
other issues, financial issues or whatever. They think I am the bill
collector. If they don’t know who you
are they aren’t going to answer the phone for you, they’re [not going to] talk
to you and frankly I don’t blame them.
You know, ‘Hi I am calling about your abnormal pap smear – you don’t
know me – that’s ridiculous!
Again, with HIPAA we
don’t leave any phone messages…. … it’s either through the mail addressed to
the patient or in person face-to-face.
We have HIPPA education, and again that is part of our orientation,
everybody has been trained in that we
have HIPPA with the DPH, in addition, with HIPPA with our providers in our
organization. So, we have very good
control on that.
The sites try to hire staff from the community to facilitate outreach and cultural competence, but some case managers emphasized that staff must be very aware of their professional responsibilities when treating their friends and neighbors.
There’s a lot of staff that work
here and live in the [neighborhood] –
and a lot of our clients are from [the same neighborhood] so you know you need
to treat someone that you see here, even if you’re a friend, like they are a
patient.
Not all sites have a private place for case managers to talk to clients. This created major problems for maintaining client confidentiality.
Everything is done in a private room with the door closed.
Because there’s so many of us in that one
little office. We do, you know close the
door, put a patient visit in progress sign up, in both English and Portuguese, “please
knock before you come in.” But some
people just don’t pay attention. It’s
hard.
It’s not right for patients to have to stand
while, you know, and fill out the forms and stuff. It’s really a tight squeeze in there
Well we have a crowded office, that’s the
only thing.
Places to talk face to face with a client -
somewhat adequate depending on what else is going on in the clinic. There’s not always space. It is really,
really hard to find places to talk, space is at a premium and if you look at my
office there are three desks and four of us in there. You know, that when… that
just, whether it is here or the health centers, uh mm there’s no space and it
is not going to get any better in the near future.”
Even access to telephones and other basic resources varied greatly:
I have a private phone, I can go behind
closed doors with a client, and have total privacy.
Everybody has their own phone line, desk.
I would say it is somewhat adequate only
because sometimes I have to wait for a line.
You know when you work for a small non-profit that never has any money,
even to get a locked filing cabinet, is huge.
Relations with Other Providers
Relations with medical providers varied depending on whether the agency doing case management was affiliated with the providers’ organization and how well WHN staff communicated with the other providers.
I would say very good,
because we do in total coordination with the doctors and what their
recommendations are. We have a central
scheduling department at the hospital and they are fabulous.… the doctor faxes
the request for what the services are to central scheduling ….like if a patient
needs to have a unilateral mammogram.
I think we have such a strong team of physicians who have contracted
with us that I think it makes it easier for us because they – between the
physician and their staff – they are very willing to help us.
One of the barriers that
we did have was that we had limited surgeons that we were contracted with and
the most popular surgeon was a woman and she has a bad habit of rescheduling
patients for their appointments so it gets very prolonged sometimes.
Times that we have the
most problem is probably at the end of the fiscal year when we’re trying to get
everything in… and I send out the doom and gloom letter to the provider saying if
it’s not in then you are not going to get paid for it; you know, we don’t know
if we’re going to have a deficiency billing and that sort thing
Staff Cultural Awareness
Interviewees were asked to assess staff awareness about cultural issues and to what degree language and culture may have caused problems for the clients in getting full benefits from the WHN program. Their self assessment was largely positive.
This is one of the most
culturally aware facilities that I’ve ever worked in.
We have a lot on staff
from different cultures because we deal with the large … multi-cultural
population
I think it works to our
advantage that the program coordinator and navigator are Portuguese.
We are very aware of
cultural differences.
Our staff tends to
mirror the population.
[A] colleague keeps up
with cultural competency committee at a hospital to understand issues re
immigrants.
In spite of these many positive comments about cultural awareness, there were others that indicated room for improvement at certain sites.
I think language is an issue because the case manager has to depend on
a community advocate to sort of be the go-between. All the contacts we had
didn’t know where the client was--ultimately she actually had a colposcopy and
it was a go-between between a clinic and a private physician’s office and she
was accessing care in both places. So
that was just a tricky case management issue and, you know, trying to get
correct information between all those sources with the patient and the program.
There are some of us who are probably more culturally aware than others.
Some of them I could say
they are … what do you call ... prejudiced.
Despite the staff diversity reflected in WHN teams at some sites, respondents highlighted a lack of diversity at other sites.
I think they could hire a more diverse
staff; although the ones that are there really know their staff….”
None of us can be culturally competent about
all the cultures that are out there. And
I think our culture right now, is one of fear and mistrust, and I think it
makes very, very hard for people who are not white or English is their first
language.
Evaluation of WHN Experience
Both clients and case managers were asked to evaluate WHN service delivery using similar fixed-response questions. In addition, case managers responded to many opportunities to comment at some length about related issues. The next section presents these data.
Overall Program Rating
Clients who had received some help from their case manager were asked to rate this help on a scale from zero to 10. These ratings can be compared to their ratings of the quality of their overall health care. As indicated in figure 7, almost one-third of the respondents rated the quality of the overall health care they had received in the past two years as a 10, while only 8% scored their health care as 6 or less on a 10-point scale. The mean health care quality score was 8.4. However, ratings of help received from the WHN case manager were even higher compared to this high level of satisfaction: 70% of clients rated the help provided by their case manager as a 10 and their mean rating was 9.5.
Figure 7
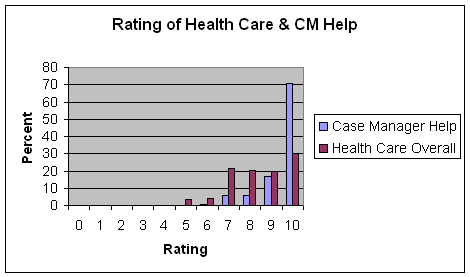
Clients’ overall impressions of the Women’s Health Network program were very positive. Two-thirds strongly agreed that they would recommend the program to a friend and almost 70% strongly agreed that they were satisfied overall with the program (table 12). Almost all agreed or strongly agreed that they were doing better because of the program. The only question that elicited some dissatisfaction concerned the program’s location, but even on this question, just 11% reported that the program’s location was not convenient for them.
Table
12
Satisfaction
with the Women’s Health Network
|
|
Would
recommend this program to a friend |
Location of
program was convenient |
Overall
satisfied with program |
Doing better
because of program |
|
Strongly agree |
75.9% |
62.9% |
68.8% |
63.9% |
|
Agree |
24.0% |
25.9% |
31.0% |
35.3% |
|
Disagree |
.1% |
10.9% |
.3% |
.6% |
|
Strongly disagree |
.0% |
.3% |
.0% |
.3% |
|
Total |
100.0% (157) |
100.0% (157) |
100.0% (157) |
100.0% (157) |
Case managers and program coordinators reported that they had received positive client feedback through thank-you cards and letters.
I have a lot of cards in one of my files
that I get from patients about my case manager – “I could not have done this
without her.”…that kind of thing.
There is a thank-you for everything you
do; not only case managed but I received a letter yesterday from a woman whom
we just saw in our clinic last week – just for her physical and her pap and her
breast exam – she comes every year – so she saw our Nurse Practitioner. She is going through some stressful times
right now in her relationship. And she
sent me a thank-you note yesterday just saying I never asked to be uninsured
but it afforded me the opportunity to meet you and Trish and to get care beyond
any expectation and I just so whole heartedly support your program. We hear that all the time.
Client and Case Manager
Ratings of Service Problems
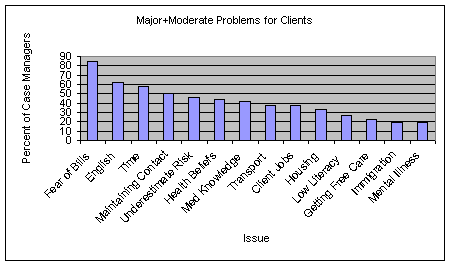
Clients were asked how much of a problem each of a series of potential barriers to receiving breast or cervical cancer screening, testing, or treatment had been for them. As indicated in Figure 8, the percentage of clients rating a problem as a moderate or major problem varied widely between potential barriers, among those who received problematic test results. Paying bills was the greatest perceived barrier, rated as a major or moderate problem by almost half of those who had received a problematic test result, and problems dealing with health insurance were also rated as a common problem. Other problems often rated as major or moderate were fear of receiving bad news and fear of the pain of testing, as well as problems in communicating in English. Distrust in the health care system and problems of time and transportation were less common.
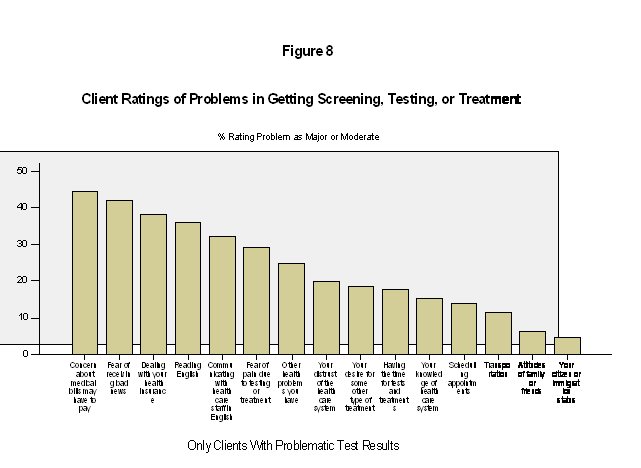
Case managers identified many of the same problems that clients did as causing problems in service delivery. Case managers rated fear of unpaid bills as the most common problem experienced by clients, as did clients themselves (figure 9). Case managers also reported that problems with English fluency were a major service problem. Other common problems reported by case managers were constraints on clients’ available time and problems of maintaining contact, as well as their clients’ particular health beliefs and limited medical knowledge. The next sections provide more detail in several of these areas.
Figure 9
Testing and Treatment
Experience
Client
Perspectives
Three-quarters of the sample reported having had at least one mammogram, one clinical breast exam, and one Pap test in their lifetime and only 7% had had no more than one of these three tests. One year had elapsed, on average, since the last such test. About one-quarter reported they had received follow-up tests indicating the possibility of cancer or were awaiting additional tests, while 14% had received test results indicating that cancer was likely.
About three-quarters reported having received some help with testing from the Women’s Health Network, although some only knew the name of the specific contracting organization that had delivered their case management services. About 60% of the clients who had received a problematic test result reported that case managers had helped with cervical cancer testing, while a total of about one-third reported having received help with breast cancer testing (table 13). Help with cervical cancer testing was much more common among those who had received a problematic test result.
Table
13
Type
of Testing by Problematic Results
|
|
Problematic
Test Result |
||
| Yes |
No |
||
|
Case manager has helped with which
type of testing |
Neither |
18.1% |
26.3% |
| Breast cancer |
21.3% |
36.8% |
|
| Cervical cancer |
48.4% |
15.8% |
|
| Both |
12.3% 100.0% (155) |
21.1% 100.0% (19) |
|
Clients who reported receiving any help in getting follow-up testing or treatment for breast or cervical cancer from a case manager rated that help very positively, particularly if they had received a problematic test result. Eighty-four percent of those who had received a problematic test result said they had received “a lot” of help (table 14).
Table 14
Help in Getting
Follow-up Testing by Problematic Results
|
|
Problematic
Test Result |
||
| Yes |
No |
||
|
How much help received |
No help |
3.1% |
.0% |
| A little help |
13.3% |
35.3% |
|
| A
lot of help |
83.6% 100.0% (128) |
64.7% 100.0% (17) |
|
The help that about 80% of clients had received from case managers included a description of follow-up tests and their possible results, whether or not they had finally received a problematic test result (table 15). Only 6.9% of those who had received a problematic test result had received from their case manager neither a description of the tests nor of their possible results; the corresponding percentage for those who had not received a problematic test result was just 11.8%.
Table
15
Case
Manager Description of Tests by Problematic Results
|
|
Problematic
Test Result |
||
|
|
Yes |
No |
|
|
Case Manager Described Tests and
Possible Results |
Neither Described |
6.9% |
11.8% |
|
|
Test or Results Described |
15.4% |
5.9% |
|
|
Both Tests & Results Described Total |
77.7% 100.0% (130) |
82.4% 100.0% (17) |
Clients who had received a problematic test result rated their treatment by the case manager very positively. Between 80 and 95% reported that their case manager had always explained follow-up testing in a way they could understand, had treated them with respect, had always listened carefully and had spent enough time with them (table 16). Clients who had not received problematic test results were similar in their ratings of their treatment by their case manager.
Table
16
Frequency
of Positive Case Management Actions
|
|
How often
did case manager explain follow-up testing services in a way you could
understand |
How often
did case manager explain listen carefully to your questions or concerns |
How often
did case manager treat you with respect |
How often
did case manager spend enough time with you |
|
Always |
82.7% |
89.2% |
94.6% |
81.4% |
|
Usually |
10.2% |
8.5% |
3.8% |
10.9% |
|
Sometimes |
5.5% |
.8% |
1.5% |
7.0% |
|
Rarely |
.0% |
.8% |
.0% |
.0% |
|
Never |
1.6% |
.8% |
.0% |
.8% |
|
Total |
100.0% (127) |
100.0% (130) |
100.0% (130) |
100.0% (129) |
About three-quarters of those who had received problematic test results reported that the case manager had provided information about follow-up testing and treatment, but information about the possible costs of that testing and treatment was reported by fewer than half (table 17). Reports were generally similar for those who had not received a problematic test result.
Table
17
Testing
and Treatment Information Case Manager Provided
|
|
Referred to
place to go for follow-up tests |
Provided
with information about details of follow-up testing |
Provided
with information about the cost of follow-up testing |
Provided
with information about the details of the treatment |
Provided
with information about the cost treatment |
|
Yes |
74.2% |
78.2% |
43.6% |
75.3% |
35.1% |
|
No |
25.8% |
21.8% |
56.4% |
24.7% |
64.9% |
|
Total |
100.0% (155) |
100.0% (156) |
100.0% (156) |
100.0% (154) |
100.0% (151) |
Levels of satisfaction with particular case management actions were high among those who had received problematic test results (table 18). Nearly all were satisfied with each case manager action and between 60 and 70% were very satisfied with these actions. Satisfaction levels were considerably lower—by 10 to 20 percentage points—among clients who had not received problematic test results.
Table 18
Satisfaction with Case
Manager Actions
|
|
Kept in touch with you |
Obtained consent |
Respect your privacy |
Helped you communi-cate with other
providers |
Provided a private place to talk |
Sensitive to your needs |
Knowledge-able answers to questions |
|
Very satisfied |
58.6% |
63.7% |
73.9% |
56.7% |
64.1% |
70.1% |
70.1% |
|
Satisfied |
33.1% |
33.8% |
24.8% |
33.8% |
29.5% |
28.0% |
25.5% |
|
Dissatis-fied |
5.7% |
1.9% |
.6% |
7.6% |
3.8% |
1.9% |
3.2% |
|
Very dis-satisfied |
2.5% |
.6% |
.6% |
1.9% |
2.6% |
.0% |
1.3% |
|
Total |
100.0% (157) |
100.0% (157) |
100.0% (157) |
100.0% (157) |
100.0% (156) |
100.0% (157) |
100.0% (157) |
Case Manager
Perspectives
Case managers highlighted clinical judgment and communication
skills, as well as adequate information systems, as crucial for helping clients
to obtain diagnostic testing and treatment.
making
sure that the patients are moved right through from, you know, screening to
diagnostic--“it’s done in a timely manner.” … the case manager can speak with
the patient, … she is always available to the patient, … should she have any
questions with regard to any clinical issues surrounding her …sub-sequential diagnosis.
[W]e handle these women pretty much the same way with really kid gloves and we
try to get them to move right through to get the services that they need. And
that is our primary focus.
if
their lab work wasn’t good and, you know, you tell them that you care and that
you need to make some changes and you talk to them about it – it’s not a five
minute phone conversation, you hang up the phone and it’s like okay … which you
get at most doctor’s offices …. Most doctors are not going to follow you that
closely. The patients love it; they feel
like they’re really cared for and for some of these women it’s the first time
that someone has cared as much.
did
anybody bother to tell them that 80% of the time … any abnormal screening
results in a benign finding? Did anybody
mention that or did they leave them frightened for 10 days? … okay …
because all they did was schedule … well, you know, the radiologist
would like you back – there’s something on your film they want a clearer view
of. … That to me is a huge strength
because we are going to take the time to tell you statistically what that means
and what an ultrasound is and if they do an ultrasound it’s non-invasive ….
Counseling a client with an abnormal test result is
complicated because of the programmatic need to discharge the client once she
has entered treatment.
I
mean that’s the kind of interesting thing about the program is that you know,
the fact that it stops at diagnosis; I mean that’s when your real work
begins. … is at diagnosis and it’s
always been a puzzle to me …. most of the activities I’ve been involved in Case
Management have been outside the realm of Women’s Health Network. It’s been after they’ve been diagnosed and
they’ve started treatment.
Everyone
I deal with has an abnormal finding so they so they just want to talk to the
nurse so to find out the ones especially worried about having cancer or they
need to go on to the next step. And the
ones that have cancer they really do need to talk it out, work it out, and I
help them get the treatment act and that doesn’t necessarily really need to be
a nurse to do it.
One of the greatest difficulties reported by case managers in
counseling clients with abnormal results was respecting clients who chose not
to follow the follow-up recommendations.
but
they don’t necessarily have to accept because they are a human being with their
own decision-making capabilities …..
By contrast, one case manager was proud of the follow-up
record of a client enrolled in the HDSPP program.
[A]
lady that we have as a client who came in quite overweight-- diabetic and
needing medication - pretty strong medication.
[She] went through risk reduction education. Followed-up and really took what we said to
heart, took the information and then stopped back in here it was like maybe 6
months later. …other than phone calls
she actually came in and had lost like 60 pounds and her sugars were under
control. That’s the best example I can
give you.
Costs
Medical costs were reported as a problem by both clients and case managers.
Client
Perspectives
Figure 10 provides more details about the problem with fear
of unpaid bills. Fewer than 40% of the
clients with a problematic test result reported that their case manager had
provided them with information about the potential costs of either testing or
treatment, although all those who had received such information were satisfied
with its accuracy. About 20% reported
that they had had to pay some of the costs associated with testing and with
treatment and at least half had had some difficulty in doing so.
Figure 10
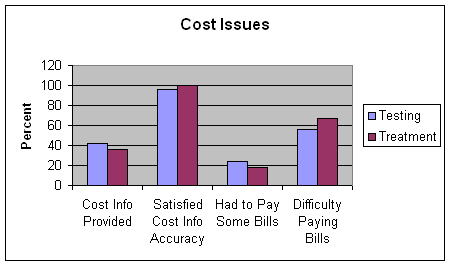
Case Manager
Perspectives
Case managers elaborated on cost issues as a barrier to effective service delivery in detailed comments. Some felt that fears of unpaid bills reflected clients’ misconceptions or fears:
It
takes a lot to get the patients to understand that this is a free service. And they are probably thinking that I’ve been
told this before. …But people have been
burned at other places where they’ve been told things were free and they
weren’t – a trust issue.
We
tell them what rights they have… Some people feel ashamed to be here without
insurance.
When people come to the health
center a lot of time their contact information is not updated. Or they don’t give it to the registration
clerk because they think it’s for billing not for lab results. So they don’t care if they miss a bill.
most of the time for that reason, you
know…. getting income verification is difficult, can be difficult. They don’t
want to give it up…. You know, I tell my
staff that it is not up to us, to… you know start digging around to find out if
people are telling us the truth or not.
If somebody is going to tell you something we have to take it as face
value. We can’t accuse people of not being truthful with you. Often they will
not give us their husband’s income, or they just tell us what they earn, you
know. We really have to, have to tread
very carefully in there, and you know that is a problem, probably more than DPH
realizes.
Other case managers reported that clients’ financial fears were too often justified:
Sometimes
they need to have services that are not covered by us. …doctors order things and they are not
covered and sometimes they don’t have the free care to pay for it. And then the treatment is very fearful. …So
you really have to help them to get reduced fees, to get the care that they
need.
Financial
counseling…[is] much much much much much much less [needed] since the Treatment
Act was passed. But it’s still
there. … had a client diagnosed with
breast cancer. …was treatment program eligible, but she wasn’t gonna be able to
work. …living hand to mouth as it was
and her question was, what if I can’t pay my rent. So where will I live and how
will I eat were the questions that came up with the last two who were
diagnosed.
DPH
sort of advertises this program as “free” breast and cervical screening and
diagnostics… well, that’s not true. It’s
free if we cover the service. There are
many services that we don’t cover… If I were the patient and I was about to go
in for something, I would want to know ahead of time, you know, what am I going
to need and what are you going to be able to cover, and what is it going to
cost me. And those are questions that we
don’t have the answers to ahead of time.
Financial
problems also frustrated case managers who wanted to take care of a broader
range of problems.
The
hard part is when we find someone and they are not eligible. Then you are doing a work around to try to
get them in and you know you are only covering a little piece of what their
problem is. You know, there are so many other needs that they have.
Our financial counselor is very overwhelmed and we’ve always wanted to
make that part of her job, to find clients and enroll them and then figure out
if they need case management.
Case managers also expressed concerns about getting their clients into the uncompensated care pool to pay for needed services not covered by WHN.
Free Care income
guidelines and ours don’t line up. Ours
is a more generous program than Free Care, so the last time we ran the
statistics about 60% of women who qualify for this program don’t qualify for
Free Care.
It’s becoming more and more difficult.
The hospital is getting more and more tight with their pool, the Free
Care pool.
Free care issues posed particular problems within the HDSPP program.
Financial restrictions of the grant are problematic. I’d like to be able to do a lot more for
people - to do more with nutrition, more with exercise. And it’s just not
available, it’s just not there.
It’s becoming very difficult because hospitals are backing off. It has to be a life threatening event for
them to qualify for Free Care. So this
is becoming a major issue, especially for the CVD patients. We are doing okay with the breast and
cervical cancer but the CVD patients, that’s a big problem.
The other issue about Free Care in a community hospital, as opposed to
a teaching hospital, is that in a community hospital Free Care only covers
services that are billed by the hospital.
It doesn’t cover physician services.
So that means if you need a cardio echogram and you come to the hospital
– well the hospital is going to pay for the echogram and that will be covered
but the cost of the cardiologist to read it is not going to be covered. Well how much does that cost? We have no way of knowing because each
cardiologist sets his own fee – so that gets very complicated. The whole issue of bills gets very
complicated.
Getting clients into treatment is also problematic for undocumented aliens, who are not eligible for the MassHealth Breast and Cervical Treatment Act. A few case managers commented on the consequences of this policy.
It [immigration status] doesn’t tend to necessarily present a problem
for us unless we need to get them into the Treatment Act.
Her immigration status definitely affected her getting on that
program. She was in our program but she
couldn’t get on the treatment program.
It’s a difficult issue and it’s one that I’ve struggled a lot with to
the point where I’ve actually considered whether we should even be screening
folks whose immigration status is different.
Because is it fair to screen them and not be able to provide them with
treatment?
Different strategies were used to help clients get as much care as possible through WHN and connect them to other covered services.
[the
case manager] explains to them the advantage of the program, especially for
people who are Free Care, you know what I mean, and so that usually is not a
problem.
Successful strategies … really educating
the financial counselors at the point of, services. Pulling them into, how we sign woman up, who
is eligible, and who isn’t.
We talk to the financial counselors and
say to them you know enroll these patients in the WHN when they are being
enrolled for uncompensated care. You
know, that’s a great way to do it. It’s
not that it’s a problem, it would be easier if it could be done that way. We’re coming around.
I think the challenges really are just
the constantly being more clear about our role is … and how we do our business
and like I said, there have been, you know, specific issues that I’ve had to
deal with that I have put across to them about procedures … that … reasons why
we don’t cover certain procedures for diagnostics …. that it seems to be in the
medical community that these things should be done … ah … but we don’t offer
them, you know … then we have to say they have to go to Free Care to get that
particular thing done. I mean some of
the docs are pretty good and just squashing it.
Language
Many comments focused on problems in service delivery based on differences in linguistic and/or cultural backgrounds. In some cases these differences were also reflected in health beliefs that impaired ongoing engagement with the WHN program.
Client
Perspectives
The language problems that clients rated as a barrier
were evident in differences in responses between
clients who were interviewed in English and those interviewed in Spanish or
Portuguese. Those who spoke Portuguese
were less likely to have heard of the Women’s Health Network and less likely to
report that it had helped them, while Spanish-speaking clients were less
satisfied with the information they had received about testing and, like
Portuguese-speakers, less satisfied with the information they had received
about treatment (figure 11).
Figure 11*
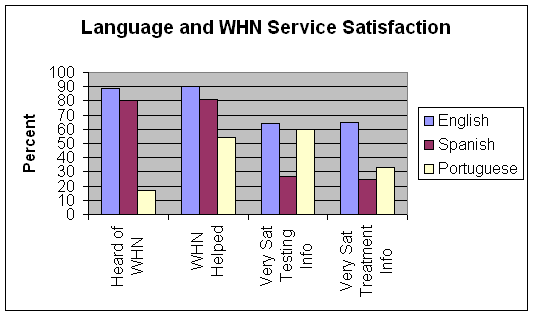
*p<.05 for all comparisons.
Women
who were interviewed in Spanish were also more likely to report several
potential barriers as a major problem, compared, in most cases, to those who
were interviewed either in English or Portuguese. Compared to both English and Portuguese
speakers, Spanish speakers rated transportation and reading English, as well as
concern with bills, family and friends’ attitudes, and their citizenship status
as more of a problem affecting their getting screening, testing or treatment
for breast or cervical cancer (figure 12).
Figure 12*
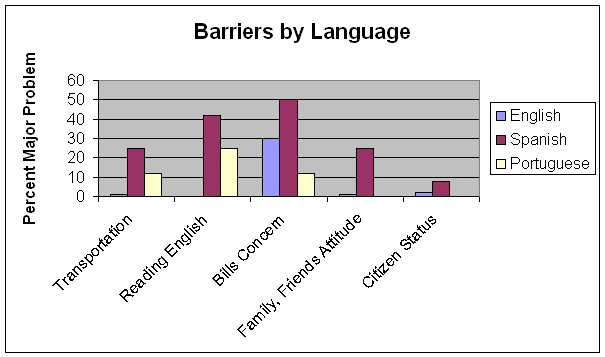 *p<.05 for all comparisons.
Percent rating potential barrier as a major problem.
*p<.05 for all comparisons.
Percent rating potential barrier as a major problem.
Case Manager
Perspectives
Case managers frequently cited language as a major barrier to program delivery and effectiveness.
They may not really understand if you don’t have somebody that is
speaking in your language. They may not
understand the importance of screening and diagnostic services.
Fluency
in English – oh good Lord that’s a major problem. And the only thing that helps us is the
interpreter.
It
can sometimes be almost half my case load.
I mean we have an interpreter but she only works for us a few hours a
week, just for like one day, and she’s not here when I’m here, so it…makes for
a lot of note writing and what I wanted to say and things like that.
Among the most frequent complaints was a lack of material in Portuguese.
Need more in Portuguese. We might not have
everything in Portuguese; I know we have things in Spanish.
We’ve had to do a lot of our own and
particularly in Portuguese ‘cause you can hardly find anything in
Portuguese. So, although we have some
things from the state, most of what we give out to the patients we’ve done.
Some case managers also felt that program materials needed to be written in simpler prose due to client literacy levels.
Just look at the English material and the literacy level is far too
high. At this point [it] should be at the third [grade] level. The last review I did the best and what I
could find was at the seventh grade level. And, unless you are an educated
person and have a diagnosis, you are never going to sit down. …beautiful,
material, beautiful, graphically pleasing, catches your eye, gorgeous, glossy,
people are putting a lot of money into it, but it is not reaching our
population at all.
Case
managers who were able to alleviate these problems commented on their methods:
The
way we’ve addressed it is that half of our staff is Portuguese speaking.
We have interpreters that go through every phase with
the client. We have an interpreter on
site at every clinic and they also go with them to the doctors’ appointments –
so that is well addressed.
Case managers also described how culture and health beliefs sometimes reduced the likelihood of follow-up.
It
is important to make sure that somebody is following them because they don’t
oftentimes view the follow-up Pap smear or that follow-up mammogram as being
important. And if we weren’t pushing
them to do it, I don’t think they would.
The
Vietnamese – they don’t like to have Pap smears.
The
Cambodian population here because they do not believe in wellness or preventive
anything in their culture and beliefs.
As a result we see very few Cambodians.
I think we saw none last year.
The
population that I’m working here doesn’t think it’s as important. They are more concerned with taking that trip
to
The
Hispanic population that we have here doesn’t tell time like we do – they are
not clock-watchers. They got there and
did their best, and trying to educate them on that is really hard. Some of the culture… think nothing of showing
up an hour late for a doctor’s appointment.
It’s socially acceptable within their group. And so they get blown away when the doctor’s
office says ‘I’m not going to see you.’
There’s
a fair amount of people who feel like why should I have this mammogram done –
if I don’t know about it, it won’t hurt me type of attitude.
Case managers at some sites felt well prepared to deal with cultural differences and alternative health views.
I
think we have a great awareness of culture here. We’re so diversified with the different
cultures that we and our employees are very aware of it.
people
just have all these cultural reasonings and think that you don’t need something
unless this happens and so that’s a lot of teaching that we do – try to get
people to understand that this is why we do it.
They
don’t believe in biopsy or that kind of stuff.
So you finally get them in and they have a mammogram… they have an
abnormal and they won’t keep going. Or
you get them through a biopsy, which is positive, and they won’t treat, because
they want to try some homeopathic or some herbs. And I totally believe in their right to feel
that way.
We’ve
had one client who returned to her native country for treatment and it is a
very poor third world country and we were very concerned that she was not going
to get the kind of treatment there that she could here. But her belief system was so strong that she
would in fact get better treatment there and also that she would have access to
alternative treatments there that she wouldn’t here …
Case
managers also expressed concern with their clients limited medical services
knowledge and underestimation of cancer or CVD risk.
They
just don’t understand what’s available for them…so often we’ll get patients
that haven’t seen a primary care physician since they had their babies – twenty
years ago!
Sometimes
you really have to drive the point home that you need to, you know, you don’t
have cancer but do have a melanoma that needs to be followed-up carefully. Don’t miss your appointments because there
could be unhealthy consequences.
The
age of the client is a huge one – the late teens, early twenties think they’re
invincible.
I
mean we have the mammogram van that comes right outside. But its tough to get people to come and I
believe it’s because people don’t really believe they are at risk and don’t
understand the importance of screening.
And the same things for Pap smears, it’s tough to get people to come in.
There
are the ones with the high blood pressure and high cholesterol and they don’t
take it seriously.
Fear and Pain
Case
managers sometimes felt that fear of finding out test results and pain
interfered with service delivery.
Our
breast cancer woman told me when she came in that she felt for a long time that
she had something wrong with her. I was
like... ‘why didn’t you,’ ‘we sent you reminders,’ ‘what could we have
done?’ She said she was afraid it was
cancer. Fear for those it affects is
huge.
It’s
usually the first one that they are so afraid of because they don’t have
anything previously to compare it to.
They are thinking okay if I do have cancer then how long have I had it –
versus well this is my second mammogram so if I do have it it’s only been since
my last – and that is a littler easier to deal with.
I
mean I have a couple of people who have problems with their breasts that
they’ve gone through a lot of mammograms and know it’s painful and they’ve
asked for valium.
My
last van date a lady came for her appointment… she went into the van, into the
tiny room and undressed and went back out.
When they told her to put her breast there so that they could smash it…
oh no… she went back in, got dressed, and came out…In her mind there was no way
she was going to put her breast in there.
Time and Scheduling Problems
Many case managers identified time and job constraints as factors that impeded service delivery:
Time
is a major problem between work schedules, kids’ school schedules, husbands or
significant others’ schedules. And the
regular business hours of the mammography center is
I
would like to be able to schedule some Saturdays for them but so far things
have not been receptive, other than the one Van date that we have here, which
is a big health fair – that’s the only Saturday that I know of that’s ever been
done here at the center.
Between April and October here
on the island it is very difficult to reach women because that’s their working
time because it is a seasonal employment.
So, employment is usually a difficult time. They don’t want to take the time. They rarely will even schedule their paps or
mammograms in the summer. And some of
our case management patients have literally told us ‘I can’t do that until the
fall’.
Some people have three jobs so
you can only reach them between
Especially
a lot of women in the Brazilian community might be working in 2 jobs,
especially anything that comes up between June and September. They are not going to want to take the time
out to go because that is when they are going to earn their money for the year.
And it is not just limited to the Brazilian community. But the Brazilian women might be working 7
days a week compared to somebody else working 5 or 6.
For
people who are working to take away their one day of getting paid, to tell them
to something that isn’t a problem – so we do our best to get around their
schedules and consolidate.
Most
of our women are working poor. And for
many of them it is a decision between food on the table or pay the doc, because
it is very hard to find a place that provides screening in the evening.
Some
of them bring their children and I will watch them for 10 minutes if that is
what it takes.
A
lot of them I notice can’t get time off from work or need a note from me, which
I think is pathetic. It is ridiculous –
you can’t take an hour here or there to take care of your health.
Some
employers don’t want them leaving their job.
Some require them to have a letter if they wanted to the leave the job –
the fear of not coming work and getting fired.
Some case managers also reported problems with the availability of medical providers for testing.
Sometimes they [providers] want
to go on vacations; it’s a little bit frustrating because they will tell you,
you know, that they are going to go away for six months and you try to tell
them that they really need to have this done and that’s a little un-nerving but
that doesn’t happen that often but I would say it happens at least once a month
that a patient says that they are not going to come back for a while. So, in general it works pretty well.
Well
as far as getting appointments here at the clinic they have limited hours cause
there is only one clinician here all week.
Limited Medical Knowledge
Clients’ limited medical knowledge was rated as creating problems for case managers who sought to deliver useful information to clients and to encourage clients to return for rescreening or treatment.
I think there are very
difficult clients who I think are going to say to me something like ‘um, I’m really
intimidated by this whole medical experience, I don’t understand that word you
just used, as a result of being a sexual abuse survivor I’m probably going to
no show for my first three colposcopies, and you are going to have to
understand I’m agoraphobic.’ …so assessment isn’t an interview. And I rely on a lot of other information in
the medical record.
I have a young woman – my age – who was
diagnosed with breast cancer three years ago in our program who did not
follow-up, did not choose to continue with the standard protocols for
treatment; not that we had the Breast Cancer Treatment Act at that time …. And she has returned and her cancer has
spread and … and I had to discharge her from case management, you know, the
three years ago and … cause she wasn’t interested in participating ….. It is
because she is a woman my age that had she participated maybe she wouldn’t be
at this point …. So she went through this again and got referred now into the
we do have one person that is slightly
mentally deficient and … ah … she came in, the doctor sent her over because she
had a lump in her breast and she was very concerned that we get it all taken
care because her insurance was running out at the end of the month ‘cause she
was laid off and so because we didn’t like the looks of it and all, she had ADA
at the time, we put her right into the program and called to make sure that
that was okay. We got her into this
program and she does have cancer.
One agency developed clear communication strategies to enlist cooperation of clients enrolled in the Heart Disease and Stroke Prevention Program:
what’s made it easier because
from the beginning they’re asked do you want to participate in this and you
know they are told what it is and will you agree to have a risk reduction
educator talk to you and then they say yes then they can get it, if they say no
they say well that’s part of it. So that’s helped a lot to try to set the tone
from the beginning. Otherwise it was so
hard for the nurse to contact these people because they know it’s an
expectation in order to have this service.
You can’t have the blood work without having the risk reduction. So that was something we started.
Transportation Problems
Case managers also described barriers due to transportation problems.
Absolutely the biggest thing
out here. It is a rural setting so
everyone lives far apart. There is no
public transportation. We have one cab
out here. I could go on and on….
We have a van service available
that helps the center but it is to and from the health center itself, not if
they have services like at a surgical office which is when we frequently run
into a problem if we’re going to.
The bus transportation could be
not on time; they are late for the appointment – they are not seen. … so their physical doesn’t get done.
We don’t have any money in the
budget for transportation.
Case managers did offer some solutions for transportation problems.
scheduling at sites that are
closer to the patient, use of shuttle systems and occasional cab vouchers
through different programs that we can get the women enrolled on.
the way we try to get around
that is, if the patient cannot find a friend (we obviously suggest those
obvious things)… outreach worker from the Y would then go up and bring them.
I’ve taken patients to
appointments, I try to work with other uh mm… people around, and you know,
whatever we can do to get people there.
Influences on Satisfaction
Satisfaction with the program was assessed in both the client phone survey and in the in-person case manager and program coordinator interviews.
Clients
Clients’ satisfaction with their WHN case management experience
varied with several personal characteristics.
Clients with more education tended to report more satisfaction with case
management (figure 13).
Figure 13
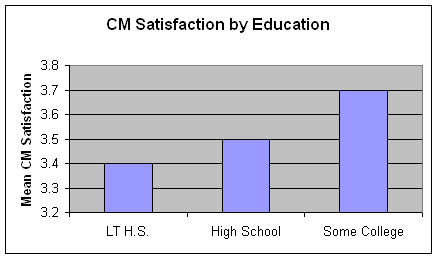
Ratings of services received also declined with clients’
ratings of their overall physical health and with their symptoms of
depression. The correlations in Table 19
indicate that satisfaction with case manager services and ratings of problems
for WHN service delivery increased with both symptoms of depression and ratings
of overall health, and general satisfaction with WHN also increased with
overall personal health rating.
Table
19
Correlations
of Satisfaction Indicators with Depression and Health
|
Symptoms of
Depression |
General
health |
||||
|
Satisfaction With Case Manager Help |
Pearson Correlation |
-.190 |
-.147 |
|
|
|
|
Sig. (2-tailed) |
.011 |
.050 |
|
|
|
|
N |
179 |
179 |
|
|
|
How Much Issues Are a Problem |
Pearson Correlation |
.275 |
.278 |
|
|
|
|
Sig. (2-tailed) |
.000 |
.000 |
|
|
|
|
N |
179 |
179 |
|
|
|
General Satisfaction with WHN |
Pearson Correlation |
-.068 |
-.170 |
|
|
|
|
Sig. (2-tailed) |
.397 |
.033 |
|
|
|
|
N |
157 |
157 |
|
|
Case Managers
Case managers’ satisfaction with their jobs tended to be positively associated with age and with the percent of clients seen at their worksite for cervical cancer, but it tended to decline with the number of clients seen face-to-face in the last month. In their comments, case managers described particular bases of satisfaction in their delivery of services to clients.
…
these patients have someone to connect with, to rely on, and to feel as though
they’re not alone – they have less to worry about maybe.
The
client contact – women who have been really hesitant and due to being pursued
quite a bit they did go get care. And
most of the time it turns out to be nothing.
But once in a while it has turned out to be something women need to take
care of.
WHN Services
Service delivery data were analyzed for all clients in case management at any point during the period studied for breast or cervical cancer issues. Fourteen percent of these 3,178 WHN clients received a problematic diagnosis indicating the likelihood of cancer and the need for further testing or treatment. The average number of clinic visits in this client population was 3.3, with an average of 15 days from the triggering event to a formal diagnosis (figure 14) and, for the 356 who were diagnosed with cancer, an average of 35 days from diagnosis to treatment (figure 15).
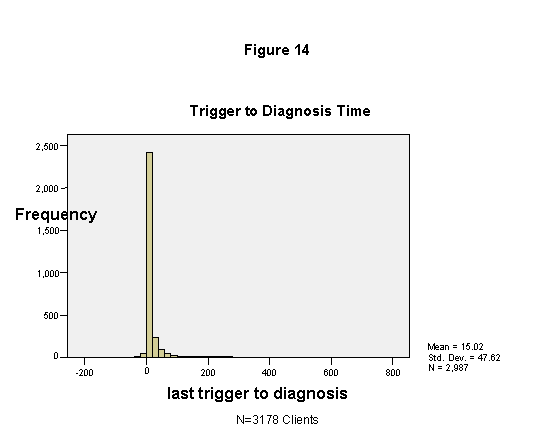
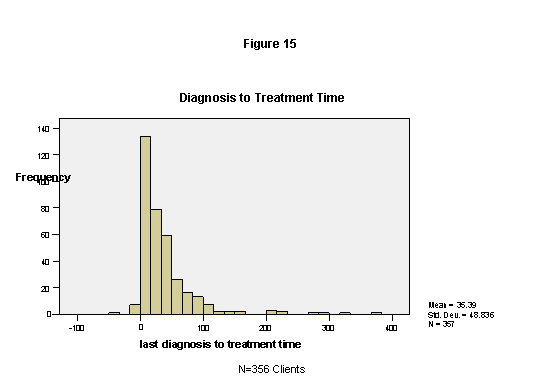
Service indicators differed with several site characteristics. The average number of clinic visits was significantly higher for the 854 clients at the sites with HDSPP services (3.6) than for the 2,324 clients at the other sites (3.2), while the average time elapsed from the triggering event to a diagnosis was slightly longer at the HDSPP sites (17.7 days) compared to the other sites (14.0 days), but the difference was not statistically significant at the .05 level. The number of clinic visits was higher, on average, for clients at the centralized medical sites (3.6) and the decentralized medical sites (3.2) than at the community health centers (2.6) and the large hospital-based collaborative (2.3) (p<.001). The average time elapsed from trigger to diagnosis was considerably elevated for the community health centers (43.6) and the large hospital-based collaborative (26.1) compared to the centralized medical sites (13.7) and the decentralized medical sites (10.2) (p<.001).
Client characteristics were also related to WHN service indicators. White (3.4) and Hispanic (3.2) clients reported more clinic visits than black clients (2.9) (p<.05) and Hispanic clients (18.1) had a longer time from the triggering event to diagnosis than either white (13.0) or black clients (13.1) (p<.05). The average number of clinic visits was significantly lower (3.1 compared to an overall mean of 3.3) for Spanish-speaking clients (p<.01) and the time from trigger to diagnosis considerably longer (20.7 compared to 14.5 overall) than for clients who spoke English or other languages (p<.001).
Disease outcomes also varied with race and with site characteristics. Eighteen percent of white clients were identified as having a test result indicating the possibility of cancer, compared to about 10% of black and Hispanic clients (p<.001). Sites with more Hispanic clients had smaller fractions of clients being seen for cervical cancer evaluation (figure 16).
Figure 16
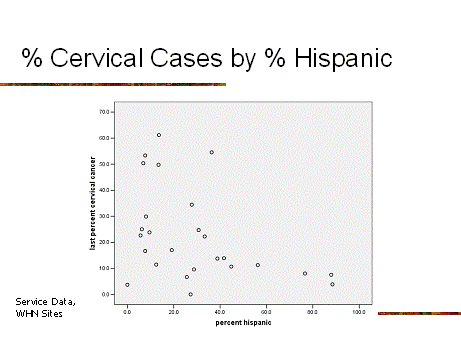
Problematic cancer results were also more common among high school graduates and those with some college (about 16%) than among those with less (10%) or more (13%) education (p<.001). Problematic cancer results were also much more common among the 429 clients in their 20s (42%) and the 334 in their 30s (16%) than among those 40 and above (about 9%) (p<.001)—presumably because women under 40 are not eligible for WHN services unless they are at high risk for breast or cervical cancer due to family history or an earlier test result. Problematic cancer results were also more likely at the decentralized sites (19%) than among the centralized medical sites (12%), the community health centers (11%), and the large hospital-based collaborative (8%) (p<.001).
Higher case manager ratings of service adequacy were associated with a shorter average time period since the last client mammogram. When case managers reported more problems in service delivery at their sites, clients tended to rate the WHN as less helpful and also had had a longer time since their last mammogram (figure 17). Clients at these sites were also less likely to be employed or in school.
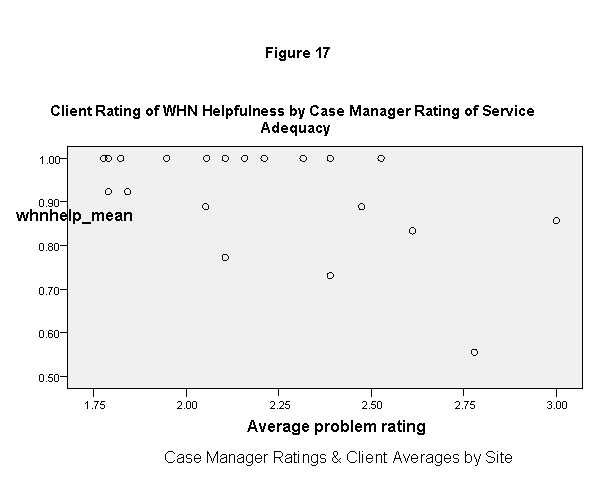
Differences Between Regions
and Contractor Types
More
detailed analyses were conducted to facilitate comparison of service delivery
in the different
All regions in the state contribute at least 10% of the total WHN client base, except for the Central region (with 5%, or N=157)), and none contribute more than 20% (the largest is the Western region, with N=623 clients). However, in these data the Metro West clients are served by only one vendor that also delivers services to women in the Northeast and Central regions. The 332 clients of this vendor are classified as “Metro West,” although their actual region is not known.
Contracting organizations were classified into four types for the analysis: Boston collaborative (consortium of community health centers for which WHN services are administered by a large hospital); decentralized sites (organizations, including visiting nurse associations, that subcontract out most WHN services to other health facilities or clinicians); centralized services (large hospitals and medical centers that provide all BCCEDP services); and community health centers (which provide services directly).
When compared to the regional distribution of uninsured, low income women in Massachusetts who are 40 to 64 years old (DHCFP Survey as reported by Kramer), the interregional differences in numbers of WHN clients suggest more effective recruitment in the Western region.
Types of contracting organizations varied between regions. Only Boston and the Central region had “community health centers” as one of their types of contracting organizations. Boston did not have any visiting nurse associations as contracting organizations, while it did contract with a large health care system that included multiple service sites in a collaborative arrangement.
Case
Characteristics
The average age
of WHN clients is higher in
Service
Delivery
Unlike the
differences in clinic visits and time until diagnosis, there was no difference
between
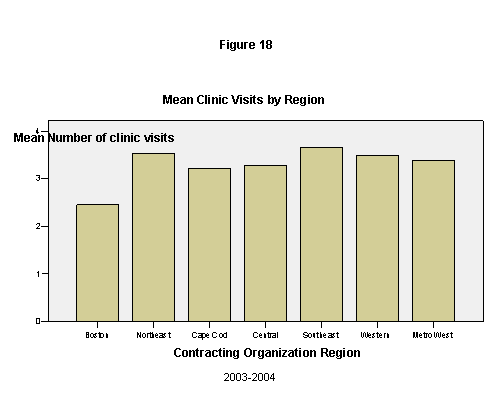
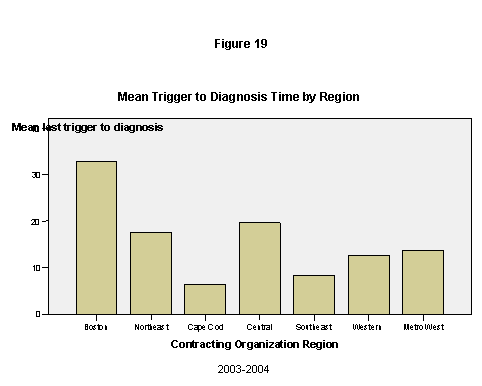
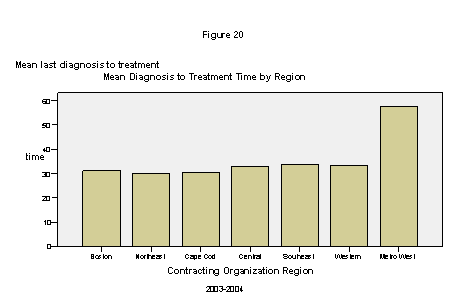
Multivariate
Analysis of Regional Differences in Service Delivery
There are three
types of contracting organizations in
The one
consistent effect of type of contracting organization between regions is that
in both regions that have community health centers—Central as well as
Women seen for breast conditions tended to have more clinic visits (3.6) and a longer time from trigger to diagnosis (16 days) than women seen for cervical conditions (2.2 visits; 11 days), but there was no consistent difference in time from diagnosis to treatment (29 days for breast cases; 38 days for cervical cases).
Multiple regression analyses that included region, vendor type, and case characteristics (diagnosis, type of cancer, race, language, education and age) as predictors explained only a small proportion of the variation in the service indicators: 8% for number of clinic visits, 4% for time from trigger to diagnosis, and 7% for time from diagnosis to treatment. The indicators of vendor type and case characteristics did not explain the regional variation in service indicators.
Controlling for
the other predictors, clinic visits were less frequent for clients seen in
Controlling for
the other predictors, time from last trigger to diagnosis was higher for
clients seen in
Controlling for the other predictors, time from diagnosis to treatment was higher for those served at the multi-site visiting nurse association and lower for Spanish-speaking clients. None of the other potential predictors examined had independent effects that were statistically significant.
Conclusions
The
case managers in the Women’s Health Network have been providing an excellent
level of service to
In spite of the very positive performance of the program overall, data from clients, case managers, and service records also indicate several aspects of service delivery that could be improved.
Both real and perceived potential testing and treatment costs diminish the likelihood of follow-up testing and treatment among clients. The difficulty of this problem is indicated in both the client and case manager survey results, although case managers indicated that the problem of treatment costs had been dramatically lessened by the recent addition of funds for treatment. Case managers provided many detailed comments about their frustrations with cost issues, including the costs that clients faced when their WHN-paid medical tests indicated other health problems for which the program does not pay. Some of these comments indicated that the scope of this problem could be lessened by providing more information about costs than is now reported by clients, but for the 20% who encounter difficulty in paying bills after their experiences with WHN, more efforts to find alternative funding sources are necessary. This was a particularly difficult for women seen in the HDSPP program, since there is no special program to cover their treatment costs, as well as for undocumented aliens.
Clients and case managers also identified language and related cultural beliefs and socioeconomic indicators as creating barriers to effective service delivery. The primary basis for this problem is the large fraction of clients who speak Spanish and Portuguese as their primary languages, compared to a case manager population that was almost exclusively Anglo and included only a few who could speak a language other than English. Both disease rates and service experiences differed by race and ethnicity and service satisfaction tended to be lower among those with less education. In general, Spanish-speaking clients seemed to be most dissatisfied, but Portuguese-speaking clients were particularly less likely to be informed about the Women’s Health Network and its services, although they were otherwise more like white clients than Spanish-speaking clients. Comments by case managers also revealed many ways in which cultural beliefs sometimes interfered with effective service delivery as well as some means for reducing this interference. Case managers indicated that translators and client navigators were important elements in the WHN response to these problems. Some case managers remarked on the need for program information to be available in Portuguese. In general, collaboration among members of the WHN service team helped case managers to respond more effectively to diverse clients.
Case managers commented at length about several other service problems and also described some strategies for lessening these problems. Lack of understanding of the importance of testing and treatment and fears about anticipated pain of testing and of finding out test results appeared to diminish follow-up by some clients. The phone survey revealed mental health problems—specifically, symptoms of depression—as a barrier to effective service delivery, but these problems were generally unacknowledged by the case managers, who rarely reported that mental health problems created another service delivery barrier.
Many case managers reported a heavy workload, particularly for those who worked more hours in their case management role and for those who worked at sites that also delivered HDSPP services. Although job satisfaction was high, particularly in terms of relations with supervisors and coworkers, case managers felt there was room for improvement in terms of salaries and the work experience itself. Some case managers described networks among service providers, particularly at hospital-based service delivery sites, as alleviating problems and many others indicated various other strategies for coping with the problems. Many case managers reported difficulties keeping in touch with clients. Women who worked long hours or who required transportation assistance presented another problem for case managers.
Case managers described many strategies to lessen the service challenges they confronted in order to maintain contact with clients, but most sought more training and better information technology support for their work.
Variability in service delivery between contracting
organizations in different regions and of different types creates a management
challenge for the Women’s Health network.
There was some indication that a larger fraction of the eligible client
pool had been reached in the Western region, while in
The case management evaluation project has provided an in-depth description of Women’s Health Network case managers, the services they provide and their clients’ evaluation of these services. Both the excellent level of service delivery that this description documents as well as the commitment demonstrated by the agency’s sponsorship of the evaluation indicate that the Massachusetts Department of Public Health’s Women’s Health Network is committed to providing even more effective service delivery in order to lessen the burden of breast and cervical cancer and heart disease in Massachusetts.
Measurement
Appendix
(1) Interviews
with all WHN case managers and program coordinators (N=52)
a.
Job experience, work roles
WHN Job Title: CURENTJB
WHN, CM hours: HRSDOCM to HRSDOOTHEROLES,
WHNHRSCHED,
WHNHRSDO,
HRSRATIO,
HRSCMDO
Interact
w Others: PCINTERACT to OTHRINTERACT
Any
CM Work: ANYCMDO
Any
Coord Work: ANYPCDO
b.
Caseload and case characteristics
Client Contact: WHNACTCASE, WHNTRIGGEVENT,
WHNSEEFACE,WHNSPKPHONE
New Clients: CASELOADD
Client Type: CLIENTPERCNTBRESTCAN,
CERVCANCER,
CMCVC
HDSPP Services: ANYCVD
Case Resolution: PRBLMTSTRESUL, DIAGCANC,
TREATPERCEN,
ENGAGCM
c.
Work activities and evaluation of them
How is Load: WKLOADDESCRIPT
WHN Task Time: Q11OFTLERNWNEED TO
OFTARRANGDISCH,
CLIENTS,
OFTSEEKADVIC TO OFTTRAIN, BRCY,
OFTFLLOWCVD TO
OFTFOLLOWGUIDELI, CVD, CLIENTRATIO,
Work Satisfaction: Q12WNEEDCM TO
ARRAGDISCHARG,
CLIENTSAT,
SEEKADVICE TO TRAINSTAFF,
BRCYSAT,
FLLOWUPCVD,FOLLOWGUIDEL, CVDSAT
Ratio of client/brc: CLIENTBSAT
Imp. of Other Dpts: NETIMPORT
Sat. Other Dpts: NETSAT
Job Factor Sat.: SATISJB TO SATIEFFECTIV, JOBSAT
d.
Problems and barriers with clients
Problem rating: PRBLMTRANS TO
PRBLMAITAINCONTAC,
PROBLEM
Service adequacy: PRBLMCONSENT TO ADQTESTR,
ADEQUACY
e.
Training and training needs
AP Nurse: AREUAPN
N Areas Trained: SUPPORTMDCAID TO
SUPPTOTHSERV,
TRAINN
Sat with Training: LEVLSATISMEDCAID TO
LEVLSATISRISKREDU,
TRAINSAT
Training
Needs: DPHTRAIN TO TIMEOFFTRAIN,
TRAINNNEED
f.
Personal characteristics
Demographics: AGE, MARITAL, DEPENDENTS, RACE
g.
Qualitative data
Interaction with Other WHN Staff
Activities and associated Barriers,
Facilitators
Problematic Issues
Adequacy of Work, Successful
Strategies
Overall WHN Effectiveness,
Barriers, Facilitators
CM Outcomes, Strengths, Challenges
Other Comments
(2) Service use
data (N=3178 clients): IDNUM,
SITE_NUMBER
|
Demographics RACETHNIC |
1-4 |
a.
|
3070 |
|
EDUCATION |
1-7 |
|
192 |
|
AGE |
|
|
|
|
Treatment
status ENROLLMENT, ENROLLMENT1, |
b.
|
c.
|
d.
|
|
ENROLLMENT2, CLNCNT, |
|
|
|
|
LAST_SERDAT |
|
|
|
|
Reason
for enrollment ISSR_REC1,
ISSR_REC2, |
e.
|
f.
|
g.
|
|
FINAL_DIAG, DIAG_REC1, |
|
|
|
|
DIAG_REC2 |
|
|
|
|
Service
Timeliness: LASTSERDAT1,LASTSERDAT2, |
h.
|
i.
|
j.
|
|
DIAG_TO_TRT2 |
|
|
|
|
TRG_TO_DIAG2 |
|
|
|
|
Tumor:
NATURE_CODE1, NATURE_CODE2, |
k.
|
l.
|
m. |
|
TUMOR_SIZE1,TUMOR_SIZE2 |
|
|
|
|
STAGE_REC1,
STAGE_REC2 |
|
|
|
|
Outcome DIAG_STAT_REC1,DIAG_STAT_REC2 |
n.
|
o.
|
p.
|
|
TRT_STATUS1, TRT_STATUS2 |
|
|
|
|
RESULT_REC1, RESULT_REC2 |
|
|
|
(3) Phone survey of random sample
of WHN B&C service recipients (N=207).
|
Overall
Health and Health Care |
Rating |
α |
N |
|
Overall health rating: Q1 |
1-5 |
|
207 |
|
Physical problems: PHYSICAL |
0-2 |
|
205 |
|
Depressed symptoms: DEPRESS |
0-2 |
.72 |
207 |
|
Insurance status: INSURED |
0,1 |
|
207 |
|
Provider connection: MEDPLACE |
0-2 |
|
207 |
|
Health Care Quality: Q9 |
0-10 |
|
207 |
|
|
|
|
|
|
Breast
and cervical exam experience |
|
|
|
|
Tests: Q10,Q12,Q14, TESTS |
0-3 |
|
207 |
|
Recency:
yrmamm,yrlumps,yrpap YEARS |
0-8.7 |
|
206 |
|
Diagnostic Status: CANCER |
|
|
|
|
Problematic Status: ANXIETY |
0-5 |
|
141 |
|
|
|
|
|
|
WHN
contact |
|
|
|
|
Know of WHN: Q16 |
0,1 |
|
201 |
|
WHN Screen/Test Help: WHNHELP |
0,1 |
|
207 |
|
Type of WHN Help: Q20a |
0-3 |
|
174 |
|
Months Since Help: TESTTIME |
.13-24 |
|
|
|
|
|
|
|
|
Satisfaction
with case manager |
q.
|
r.
|
s.
|
|
Help Received: Q22, CMDESCRIBE |
1-3 0-2 |
.64 |
145 147 |
|
Good Relation Frequency: FREQ |
1-5 |
.83 |
147 |
|
Rating of CM Help: Q29 |
0-10 |
|
147 |
|
Info Provided: CMINFO |
0-5 |
.69 |
179 |
|
Satisfaction with Info: Q40a,Q41a,Q42b, Q43a,Q44b INFOSAT |
1-4 |
.91 |
165 |
|
Costs: Q42,Q42a,Q42b,
Q43,q43A, |
|
|
|
|
q44,q44a,q44b, PAID |
0-2 |
|
159 |
|
Sat with details: Q45a to Q45G, |
|
|
|
|
CMSAT |
1-4 |
.91 |
179 |
|
Barriers
to testing or treatment |
|
|
|
|
Q46 to Q60, PROBLEMS |
1-4 |
.77 |
179 |
|
Evaluation
of WHN |
|
|
|
|
Q6164@61 to Q6164@64,
WHNSAT |
1-4 |
.84 |
157 |
|
|
|
|
|
|
Personal
characteristics |
|
|
|
|
Marital Status: MARRIED |
|
|
|
|
Work/Student Status: BUSY,
Q68 |
0-2 |
|
205 |